Intrauterine growth retardation
Definition
The term intrauterine growth retardation (also known as intrauterine growth restriction)(IUGR) is generically defined as a fetus who is at or below the tenth percentile in weight for its gestational age. There are two factors necessary to define an IUGR fetus: first, the fetal weight is at or below the tenth percentile for gestational age and sex; second, there is a pathological process present that prevents expression of normal growth potential. If the baby is small given its in utero age, then it is said to be small for gestational age (SGA).
Description
There are standards or averages in weight for unborn babies according to their gestational age in weeks; however, using a fetal growth curve derived from one population and applying it to another can result in over- or underestimation of the true incidence of SGA. For example, the lowest mean birth weight has been noted in Africa (New Guinea Lumi's tribe: mean birth weight = 2,400 grams); whereas the largest mean birth weight has been noted in the Caribbean (Aguilla: mean birth weight = 3,880 g). A population of smaller individuals will have smaller babies, so the difference lies in the genetic growth potential.
The normal intrauterine growth pattern occurs in three stages. In the first stage, four to 20 weeks gestation, rapid cell division and multiplication (hyperplasia) occurs as the embryo grows into a fetus. In the second stage, 20–28 weeks gestation, cell division (hyperplasia) declines and the cells increase in size (hypertrophy). In stage three, 28–40 weeks, there is a rapid increase in cell size, rapid accumulation of fat, muscle, and connective tissue. Ninety-five percent of fetal weight gain occurs during the last 20 weeks of gestation. If the delicate process of development and weight gain is disturbed or interrupted, the baby can suffer from restricted growth.
IUGR is usually classified as symmetrical or asymmetrical. Growth inhibition during the first stage produces an undersized fetus with fewer cells, but normal cell size, causing symmetric IUGR. In symmetrical IUGR weight, head and length are all below the tenth percentile and the baby's head and body are proportionately small. Conditions associated with symmetric IUGR include: genetic (constitutional, chromosomal and single gene defects, and deletion disorders and inborn errors of metabolism), congenital anomalies, intrauterine infections, and therapeutic irradiation. Substance abuse and cigarette smoking , depending on dose and timing, can cause either symmetrical or asymmetrical IUGR.
Growth inhibition during stage two and three causes a decrease of cell size and fetal weight with less effect on total cell number and fetal length and head circumference, causing asymmetric IUGR. Conditions associated with asymmetric IUGR include: uteroplacental insufficiency, which is usually caused by chronic hypertension or preeclampsia; chronic renal disease; cyanotic heart disease; hemoglobinopathies; placental infarcts; abruptio placenta; multiple gestation; velamentous insertion of the umbilical cord and circumvallate placenta; and high altitude. In asymmetrical IUGR, weight is below the tenth percentile, and head and length are preserved. The brain can weigh five or six times more than the liver, whereas in a normal infant, the brain weighs about three times more than the liver.
Causes and symptoms
The two types of IUGR described previously contribute to IUGR according to the development at that stage. Symmetrical IUGR may occur when the unborn baby experiences a problem during early development. Asymmetrical IUGR may occur when the unborn baby experiences a problem during later development. In general, most physicians believe that IUGR is the consequence of a disease process within one or more of the three partitions that maintain and regulate fetal growth, i.e., the maternal compartment, the placenta, or the fetus.
In consideration of risk factors uteroplacental insufficiency contributes to 80 percent of IUGR due to the following maternal causes:
- deficient supply of nutrients
- smoking
- malnutrition
- anemia
- drug abuse
- vascular diseases, i.e., high blood pressure
- chronic kidney disease
- severe diabetes
- multiple gestation
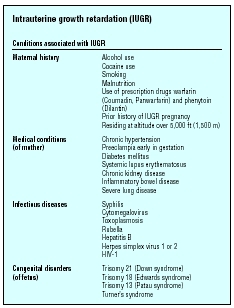
| Conditions associated with IUGR | |
| Maternal history |
Alcohol use
Cocaine use Smoking Malnutrition Use of prescription drugs warfarin (Coumadin, Panwarfarin) and phenytoin (Dilantin) Prior history of IUGR pregnancy Residing at altitude over 5,000 ft (1,500 m) |
| Medical conditions (of mother) |
Chronic hypertension
Preeclampia early in gestation Diabetes mellitus Systemic lupus erythematosus Chronic kidney disease Inflammatory bowel disease Severe lung disease |
| Infectious diseases |
Syphilis
Cytomegalovirus Toxoplasmosis Rubella Hepatitis B Herpes simplex virus 1 or 2 HIV-1 |
| Congenital disorders (of fetus) |
Trisomy 21 (Down syndrome)
Trisomy 18 (Edwards syndrome) Trisomy 13 (Patau syndrome) Turner's syndrome |
- antigen/antibody reactions, i.e., lupus, antiphospholipid antibody syndrome (APA)
- primary placental causes, i.e., extensive placental infarctions, chronic placental separation, placenta previa
Primary fetal causes contribute to 20 percent of IUGR and include the following:
- exposure to an infection, i.e., rubella (German measles ), cytomegalovirus, syphilis, or toxoplasmosis
- birth defects, i.e., congenital heart disease , genitourinary anomalies, central nervous system defects
- chromosomal abnormalities, i.e., trisomy 13, 18, or 21
- primary bone or cartilage disorder
- decreased intrinsic growth, symmetrical IUGR
Diagnosis
IUGR can be difficult to diagnose but it begins with taking an extensive maternal history. A mother with a previous IUGR is at risk of having another during a subsequent pregnancy. Maternal renal and cardiopulmonary disease and multiple gestation are factors in IUGR. A positive rollover test is predictive of IUGR and is defined as a rise in diastolic blood pressure of 20 mm Hg or more with a position change from the left lateral recumbent to supine, which is an early indication of possible pregnancy-induced hypertension. Determination of an accurate due date is essential in order for the doctor to know if development and weight gain are appropriate. Checking the mother's weight and abdominal measurements can help diagnose cases in which there are no other risk factors present. During each prenatal visit, the healthcare provider uses a tape measure to record the uterine fundal height (measured from the top of the pubic area to the top of the uterus in centimeters). As the pregnancy continues and the baby grows, the uterus stretches upward in the direction of the mother's head. Between 20 and 34 weeks gestation, the uterine fundal height, in centimeters, equals the weeks of gestation. If the uterine fundal height is more than three to four below normal, IUGR is suspected. Ultrasound is used to evaluate the growth of the baby and the ratio of the head circumference (HC) to the abdominal circumference (AC) is a good predictor of asymmetric IUGR. Decreased amniotic fluid (oligohydramnios) is associated with IUGR as the fetus may have a decreased cardiac output and thus decreased renal flow to produce less urine. The grading of the placenta indicates whether it may be inappropriately aging, but this is not as accurate as fetal measurements. Doppler flow studies of the uterine artery provide information regarding the blood flow to the uterus. Doppler studies on the umbilical cord artery and the middle cerebral artery also provide information regarding fetal growth. Biochemical tests on hormone levels of estriol and human placental lactogen provide minimal information.
Treatment
Maternal bed rest is the initial approach for the treatment of IUGR. The benefit of bed rest is that it results in increased blood flow to the uterus. Studies on the efficacy of bed rest have been inconclusive, although in the early 2000s it is still used in combination with intravenous fluid therapy and oxygen therapy. The use of baby aspirin therapy remains controversial but theoretically it serves to preserve or improve blood flow to the placenta. If the baby does not grow well in utero after conservative treatment, an obstetrician may suggest inducing labor in the mother a few weeks early, or delivering the baby by cesarean section .
KEY TERMS
Abruptio placentae —Premature separation of the placenta from the uterine wall. It occurs late in pregnancy and results in bleeding that may or may not establish an obstetrical emergency.
Circumvallate placenta —The existence of a thick, round, white, opaque ring around the periphery of the placenta that limits the expansion of the fetal vessels.
Fundus —The inside of an organ. In the eye, fundus refers to the back area that can be seen with the ophthalmoscope.
Hemoglobinopathies —Abnormal hemoglobins in the blood, i.e., sickle cell disease, thalessemia.
Hyperplasia —A condition where cells, such as those making up the prostate gland, rapidly divide abnormally and cause the organ to become enlarged.
Hypertrophy —An increase in the size of a tissue or organ brought about by the enlargement of its cells rather than cell multiplication.
Hypoplasia —An underdeveloped or incomplete tissue or organ usually due to a decrease in the number of cells.
Placenta —The organ that provides oxygen and nutrition from the mother to the unborn baby during pregnancy. The placenta is attached to the wall of the uterus and leads to the unborn baby via the umbilical cord.
Placenta previa —A condition in which the placenta totally or partially covers the cervix, preventing vaginal delivery.
Placental infarction —An area of dead tissue in the placenta that is due to an obstruction of circulation in the area.
Preeclampsia —A condition that develops after the twentieth week of pregnancy and results in high blood pressure, fluid retention that doesn't go away, and large amounts of protein in the urine. Without treatment, it can progress to a dangerous condition called eclampsia, in which a woman goes into convulsions.
Uteroplacental insufficiency —Designates the lack of blood flow from the uterus to the placenta, resulting in decreased nourishment and oxygen to the fetus.
Velamentous insertion of the umbilical cord —The attachment of the umbilical cord close to the membranes (bag of water) or in the membranes.
Prognosis
Outcomes for infants with IUGR differ depending on whether the condition is symmetrical or not and whether there are other sequelae from the underlying cause of the IUGR. Outcomes include an increased risk of long-term neurologic and behavioral handicaps, possible intrauterine demise, low blood sugar ( hypoglycemia ), and low body temperature (hypothermia). These risks increase with the severity of the growth restriction. The growth that occurs after birth cannot be predicted with certainty based on the size of the baby when it is born. Infants with asymmetrical IUGR are more likely to catch up in growth after birth than are infants who suffer from prolonged symmetrical IUGR. Delayed eruption of teeth and enamel hypoplasia and an increased incidence of postnatal infections are frequently seen. Each case is unique. Some infants who have IUGR develop normally, while others have complications of the nervous system or intellectual problems such as learning disorders . If IUGR is related to a disease or a genetic defect, the future of the infant is related to the severity and the nature of that disorder.
Parental concerns
Pregnant women who have been diagnosed with a fetus with IUGR should talk to their obstetrician about options for treatment. If the woman is uncomfortable with options presented by the doctor, she should seek a qualified second opinion. All pregnant women are well-advised to eat properly, get enough rest, and refrain from alcohol, drugs, and tobacco use for the health of the infant. In addition, pregnant women should be especially careful to keep themselves healthy by following good hygiene practices and receiving a flu vaccine if one is recommended.
Resources
BOOKS
Cunningham, F. Gary, et al. Williams Obstetrics , 21th ed. Stamford, CT: Appleton & Lange, 2002.
Olds, Sally, et al. Maternal-Newborn Nursing & Women's Health Care , 7th ed. Saddle River, NJ: Prentice Hall, 2004.
ORGANIZATIONS
American College of Obstetricians and Gynecologists. 409 12th Street, SW, PO Box 96920, Washington, DC 20090. Web site: http://www.acog.org.
Association of Women's Health, Obstetric and Neonatal Nursing. 2000 L Street, NW Suite 740, Washington, DC 20036. Web site: <www.awhonn.org.
Linda K. Bennington
Comment about this article, ask questions, or add new information about this topic: