Pneumonia
Definition
Pneumonia is an infection of the lungs that can be caused by nearly any class of organism known to cause human infections, including bacteria, viruses, fungi, and parasites. It results in an inflammatory response within the small air spaces of the lung (alveoli).
Description
Pneumonia can develop gradually in children after exposure to the causative organism, or it can develop quickly after another illness, reducing the lungs' ability to receive and distribute oxygen. It can be mild and easily cured with antibiotics and rest, or it can be severe and require hospitalization . The onset, duration, and severity of pneumonia depend upon the type of infective organism invading the body and the response of the child's immune system in fighting the infection. Respiratory distress represents 20 percent of all admissions of children to hospitals, and pneumonia is the underlying cause of most of these admissions.
To understand pneumonia, it is important to understand the basic anatomic features of the respiratory system. The human respiratory system begins at the nose and mouth, where air is breathed in (inspired) and out (expired). The nasopharynx is the air tube extending from the nose that directs air into the lungs. Air breathed in through the mouth travels through the oropharynx, which also carries swallowed food, water, and salivary secretions through the food tube (esophagus) and then into the stomach. The nasopharynx and oropharynx merge into the larynx, which is protected by a trap door called the epiglottis. The epiglottis normally prevents substances that have been swallowed, as well as substances that have been regurgitated (vomited), from heading down through the larynx into the lungs.
The larynx flows into the trachea, which is the broadest part of the respiratory tract. The trachea divides into the right and left bronchi, each branching off into multiple smaller bronchi that course throughout the lung tissue. Each bronchus divides into tubes of smaller and smaller diameter, finally ending in the terminal bronchioles. The alveoli, in which oxygen and carbon dioxide are exchanged, are clustered at the ends of the bronchioles. Lung stroma, the tissue of the lung, serves a supportive role for the bronchi, bronchioles, and alveoli.
The main function of the respiratory system is to help distribute oxygen, the most important energy source for the body's cells. Oxygen enters the body as inspired air and travels through the respiratory system to the alveoli. The oxygen is then picked up by hemoglobin, the oxygen-carrying protein in red blood cells, and delivered throughout the body through the circulatory system. Oxygen in the inspired air is exchanged within the alveoli of the lungs for carbon dioxide, a waste product of human metabolism. Carbon dioxide leaves the lungs during expiration.
The healthy human lung is sterile, with no normally resident bacteria or viruses, unlike the upper respiratory system and parts of the gastrointestinal system, where bacteria dwell even in a healthy state. Multiple safeguards along the path of the respiratory system are designed to keep invading organisms from causing infection. The first line of defense includes tiny hairs in the nostrils that filter out large particles. The epiglottis helps prevent food and other swallowed substances from entering the larynx and the trachea. Sneezing and coughing, both provoked by the presence of irritants within the respiratory system, help to clear such irritants from the respiratory tract. Mucus produced through the respiratory system also serves to trap dust and infectious organisms. Tiny hair like projections (cilia) from cells lining the respiratory tract beat constantly to move debris trapped by mucus upwards and out of the respiratory tract. This mechanism of protection is referred to as the mucociliary escalator. Finally, cells lining the respiratory tract produce several types of immune substances that protect against various organisms. Other cells (macrophages) along the respiratory tract surround and kill invading organisms.
Organisms that cause pneumonia, then, are usually prevented from entering the lungs by virtue of these host defenses. However, when a large number of organisms are encountered at once or when the immune system is weakened, the usual defenses may be overwhelmed and infection may occur. This can happen either by inhaling contaminated air droplets or by the aspiration of organisms inhabiting the upper airways. Aspiration pneumonia is a type of pneumonia in which something is aspirated from the upper airway into the lungs. This can be food from the mouth, a foreign object or substance that has entered the mouth, or regurgitated stomach contents (vomitus) aspirated into the lungs as it travels to the mouth.
The invading organism causing pneumonia provokes an immune response in the lungs that causes inflammation of the lung tissue (pneumonitis), a condition that actually makes the lung environment more ideal for infection. Small blood vessels in the lungs (capillaries) begin to empty protein-rich fluid into the alveoli, a condition that results in a less functional area for oxygen-carbon dioxide exchange. The individual becomes relatively oxygen deprived, while retaining potentially damaging carbon dioxide. This results in rapid respiration (tachypnea or faster and faster breathing) in an effort to bring in more oxygen and blow off more carbon dioxide.
Consolidation, a feature of bacterial pneumonia, occurs when the alveoli, which are normally hollow air spaces within the lung, instead become solid due to quantities of fluid and debris. Viral pneumonias and mycoplasma pneumonias do not result in consolidation. These types of pneumonia primarily infect the walls of the alveoli and the stroma of the lung. Bacterial and viral pneumonia occur mostly in winter months, while mycoplasma pneumonia is more common in summer and fall.
Bacterial pneumonia develops after the child inhales or aspirates pathogens. Viral pneumonia stems primarily from inhaling infected droplets from the upper airway into the lungs. In neonates, pneumonia may result from colonization of the infant's nasopharynx by organisms that were in the birth canal at the time of delivery.
In addition to exposure to sufficient quantities of causative organisms, certain other conditions can increase the risk of pneumonia. These include the following:
- abnormal anatomical structure, particularly of the chest or lungs
- cigarette smoke, inhaled directly by a smoker or second-hand
- immune system deficiencies ( common variable immunodeficiency , immunoglobulin deficiency syndromes , HIV infection , and others)
- swallowing difficulties as a result of stroke or seizures
- intoxication by alcohol and drugs that may interfere with normal cough reflex and decrease the chance of clearing unwanted debris from the respiratory tract
- viruses that may interfere with ciliary function, allowing themselves or other invading microorganisms such as bacteria access to the lower respiratory tract
- various chronic conditions such as asthma , cystic fibrosis , diabetes, emphysema, and neuromuscular diseases that may interfere with the seal of the epiglottis
- advanced age and associated immune system weakness
- esophageal disorders that may result in stomach contents passing upwards
- genetic factors and associated changes in DNA
- post-operative complications including the use of certain therapeutic drugs, suppressed cough reflex, breathing difficulties, and pain at the surgical site that affects breathing
- malnutrition
- radiation treatment for breast cancer , which may weaken lung tissue
The epidemic of immmunodeficiency virus (HIV), the virus that causes acquired immunodeficiency syndrome ( AIDS ), has resulted in a huge increase in the incidence of pneumonia. Because AIDS results in immune system suppression, individuals with AIDS are highly susceptible to all kinds of pneumonia, including some previously rare parasitic types that would not cause illness in someone with a normal immune system.
Pneumonia is also the most common fatal infection acquired by already hospitalized patients. Even in nonfatal cases, pneumonia is a significant economic burden on the healthcare system. One study estimates that U.S. workers who develop pneumonia cost employers five times as much in health care as the average worker.
Transmission
Pneumonia is not usually passed from one person to another. The bacterial and viral organisms that cause pneumonia, however, can be transmitted through airborne or direct contact.
Demographics
Every year in the United States, two million people of all ages develop pneumonia, including 4 percent of all the children in the country. It is the sixth most common disease leading to death and the fourth leading cause of death in the elderly; 40,000 to 70,000 people die from pneumonia each year. The incidence of pneumonia in children younger than one year of age is 35 to 40 per 1,000; 30 to 35 per 1,000 children ages two to four; and 15 per 1,000 children between ages five and nine. Fewer than 10 children in 1,000 over age nine are reported to develop pneumonia. The Centers for Disease Control and Prevention (CDC) reports that the number of deaths from pneumonia in the United States declined between 2001 and 2004.
Causes and symptoms
The list of organisms that can cause pneumonia is lengthy and includes nearly every class of infecting organism: viruses, bacteria, bacteria-like organisms, fungi, and parasites (including certain worms). Different organisms are more frequently encountered by different age groups, and other individual characteristics may increase risk for infection by particular types of organisms:
- Viruses cause the majority of pneumonias in young children, especially respiratory syncytial virus, parainfluenza and influenza viruses, and adenovirus.
- Adults are more frequently infected with bacteria such as Streptococcus pneumoniae , Haemophilus influenzae , and Staphylococcus aureus .
- Pneumonia in older children and young adults is often caused by the bacteria-like Mycoplasma pneumoniae , the cause of pneumonia that is often called "walking" pneumonia.
- Pneumocystis carinii causes pneumonia in immunosuppressed individuals such as patients being treated with chemotherapy or people with AIDS. Classically considered a parasite, it appears to be more related to fungi.
- Chlamydia psittaci can be infective in some individuals, such as poultry farm workers, who have direct contact with bird droppings.
Pneumonia is suspected in a child who has symptoms such as fever , cough, chest pain, difficulty breathing (shortness of breath or dyspnea), and an increased number of breaths per minute (respiration). Fever with a shaking chill is even more suspicious. Mucus production is typically increased and leaky capillaries in the lungs may tinge the mucus with blood. The alveoli fill further with fluid and debris from the large number of white blood cells being produced to fight the infection. Children may cough up clumps of sputum or phlegm, secretions produced in the alveoli during the infection or inflammatory condition. These clumps may appear streaked with pus or blood. In severe pneumonia, mucus plugs and the accumulation of fluid together decrease the efficiency of gas exchange in the lung, resulting in signs of oxygen deprivation. Reduced oxygen levels in the blood may produce a blue appearance of the nail beds or lips (cyanosis).
Diagnosis
Diagnosis is based on the parents' report of the onset of illness and the symptoms that have developed, combined with examination of the chest. Physical examination may indicate labored breathing. Listening with a stethoscope may reveal abnormal crackling sounds (rales), and tapping on the back, which normally yields a resonant sound due to air filling the alveoli, may yield a dull thump if the alveoli are filled with fluid and debris.
Laboratory diagnostic tests may include staining sputum samples on a glass slide and looking at the stained specimen under a microscope to determine if white cells, red cells, or bacteria are present. Identification of the specific type of bacteria may require culturing the sputum, a microbiological technique that identifies disease-causing bacterial organisms in infected material. A small sample of sputum will be streaked on a special plate filled with medium that allows the specific organism to be grown in the laboratory under certain conditions. The bacteria can then be identified and, by performing antibiotic sensitivity tests on the bacteria, appropriate treatment can usually be prescribed. In addition, oxygen and carbon dioxide levels may be measured (blood gases) and the exchange evaluated (oximetry).
If pneumonia is present, a rapid rate of respiration may be noted; tachypnea is defined as a respiratory rate over 50 respirations per minute in infants younger than
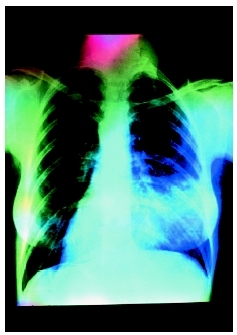
X-ray examination of the chest may reveal certain abnormal changes associated with pneumonia. Localized shadows obscuring areas of the lung may indicate a bacterial pneumonia, while streaky or patchy changes in the x-ray film may indicate viral or mycoplasma pneumonia. These changes on x ray, however, are known to lag in time behind actual symptoms.
Treatment
Prior to the discovery of penicillin and other antibiotics, bacterial pneumonia was almost always fatal. In the early 2000s, especially given early in the course of the disease, antibiotics are very effective against bacterial causes of pneumonia. Penicillin was, as of 2004, still the first choice for treating children with pneumonia unless the child is known to be penicillin-resistant. Oral amoxicillin or cephalosporins are often administered first in treating milder cases of pneumococcal pneumonia in children younger than age five, though they are not used in newborns. Erythromycin and tetracycline are broad-spectrum antibiotics that are known to improve recovery time for symptoms of mycoplasma pneumonia. They do not, however, eradicate the organisms. If the results of culture and sensitivity positively identify the causative bacteria, an antibiotic is prescribed for that demonstrated sensitivity. Viruses do not usually respond to antibiotics. Amantadine and acyclovir may be helpful against certain viral pneumonias.
Linezolid (Zyvox), the first of a new line of antibiotics known as oxazolidinones, is used to treat penicillin-resistant organisms that cause pneumonia. Another newer drug known as ertapenem (Invanz) is reported to be effective in treating bacterial pneumonia.
The child is also be given fluids and possibly drug therapy to thin mucus secretions (mucolytic agents) or medication to open the airways of the lung (brochodilators). Cough suppressants may be given as well as pain medication and fever-reducing medication. Hospitalized children may receive extra oxygen, respiratory therapy, and intravenous antibiotics and fluids.
Alternative treatment
Vitamin C is known to improve immune response and to help reduce inflammation. Grape seed extract enhances immune system functioning and helps protect lung tissue. These are adjunctive measures that do not destroy the causative organism as antibiotics do. Although garlic and certain herbs such as yerba mansa may have antibiotic properties, they cannot replace specific antibiotics used to treat pneumonia.
Prognosis
Prognosis varies according to the type of organism causing the infection, the status of the immune system, and the overall health of the affected child. Generally, there are lower mortality rates from pneumonia in the United States than elsewhere in the world. Streptococcus pneumoniae , the most common organism causing pneumonia, has a significantly lower death rate of about 5 percent. More complications occur in the very young or very old with multiple areas of the lung infected simultaneously. The presence of chronic illnesses such as diabetes, cirrhosis, and congestive heart failure may increase the chance of complications. Individuals with immunodeficiency disorders, various types of cancer, or AIDS are also more prone to complications. In children, cystic fibrosis, aspiration problems, immunodeficiencies, and congenital or acquired lung malformation may increase the risk of pneumonia from S. pneumoniae.
KEY TERMS
Alveoli —The tiny air sacs clustered at the ends of the bronchioles in the lungs in which oxygen-carbon dioxide exchange takes place.
Aspiration —The process of removing fluids or gases from the body by suction. Also refers to the inhalation of food or liquids into the lungs.
Cilia —Tiny hairlike projections on certain cells within the body. Cilia produce lashing or whipping movements to direct or cause motion of substances or fluids within the body. Within the respiratory tract, the cilia act to move mucus along, in an effort to continually flush out and clean the respiratory tract.
Consolidation —A condition in which lung tissue becomes firm and solid rather than elastic and air-filled, arising because of accumulated fluids and tissue debris.
Culture —A test in which a sample of body fluid is placed on materials specially formulated to grow microorganisms. A culture is used to learn what type of bacterium is causing infection.
Cyanosis —A bluish tinge to the skin that can occur when the blood oxygen level drops too low.
Pneumocystis carinii —An organism that causes pneumonia in immunodeficient individuals, such as people with AIDS.
Respiratory system —The organs that are involved in breathing: the nose, the throat, the larynx, the trachea, the bronchi and the lungs. Also called the respiratory tract.
Sputum —The substance that is coughed up from the lungs and spit out through the mouth. It is usually a mixture of saliva and mucus, but may contain blood or pus in patients with lung abscess or other diseases of the lungs.
Stroma —A term used to describe the supportive tissue surrounding a particular structure. An example is the tissue that surrounds and supports the actually functional lung tissue.
Tachypnea —Rapid breathing.
Recovery following pneumonia with Mycoplasma pneumoniae is nearly 100 percent. However, in the very young or very old or immunodeficient, Staphylococcus aureus has a death rate of 30 to 40 percent. Similarly, infections with a number of gram negative bacteria (such as those in the gastrointestinal tract that can cause infection following aspiration) have a death rate of 25 to 50 percent.
Prevention
Because many bacterial pneumonias occur in people who were first infected with the influenza virus (the flu), yearly flu vaccinations can decrease the risk of pneumonia for the elderly and children or adults with chronic diseases such as asthma, cystic fibrosis, other lung or heart diseases, sickle cell anemia , diabetes, kidney disease, and cancer.
A specific vaccine against Streptococcus pneumoniae can be protective for people with chronic illnesses.
Immunodeficient individuals are at higher risk for infection with Pneumocystis carinii and are frequently put on a regular preventive drug regimen of trimethoprim sulfa and/or inhaled pentamidine to avoid pneumocystis pneumonia.
Parental concerns
Pneumonia in a child can produce severe symptoms that can be frightening to both the child and parents, particularly when breathing is compromised or cyanosis is noted. When symptoms seem to suggest pneumonia, immediate attention allows early treatment so that breathing difficulties can be corrected quickly and drug therapy begun in order to destroy the causative organism. Parents can try to reassure young children and keep them as calm as possible, knowing that anxiety also increases breathing difficulties.
See also Common variable immunodeficiency .
Resources
BOOKS
"Pneumonia." Section 6, Chapter 73 in The Merck Manual of Diagnosis and Therapy , edited by Mark H. Beers and Robert Berkow. Whitehouse Station, NJ: Merck Research Laboratories, 2003.
ORGANIZATIONS
American Lung Association. 1740 Broadway, New York, NY 10019. Web site: http://www.lungusa.org.
Centers for Disease Control and Prevention. 1600 Clifton Rd., NE, Atlanta, GA 30333. Web site: http://www.cdc.gov.
WEB SITES
Cantu, Santos, Jr. "Pneumonia, Mycoplasma." eMedicine , July 13, 2001. Available online at http://www.emedicine.com/EMERG/topic467.htm (accessed November 22, 2004).
National Heart Lung and Blood Institute (NHLBI), Available online at http://www.nhlbi.nih.gov (accessed November 22, 2004).
L. Lee Culvert Rosalyn Carson-DeWitt, MD Rebecca J. Frey, PhD
Comment about this article, ask questions, or add new information about this topic: