Diaper rash
Definition
Dermatitis of the buttocks, genitals, lower abdomen, or thigh folds of an infant or toddler is called diaper rash. The outside layer of skin normally forms a protective barrier that prevents infection; when the barrier fails, the child may develop a rash in the area covered by the diaper. Diaper rashes occur equally with cloth diapers and disposable diapers.
Description
Diaper dermatitis results from prolonged contact with irritants such as moisture, chemical substances, and friction. Urine ammonia, formed from the breakdown of urea by fecal bacteria, is irritating to sensitive infant skin. Ammonia by itself does not cause skin breakdown. Only skin damaged by infrequent diaper changes and constant urine and feces contact is prone to damage from ammonia in urine. Inadequate fluid intake, heat, and detergents in diapers aggravate the condition. Bouts of diarrhea can quickly cause rashes in most children. Diaper rash begins with erythema in the perianal region. Left untreated, the area can quickly excoriate and progress to macules and papules, which form erosions and crust. Under certain circumstances (in infants under the age of six months, toddlers who have been on antibiotics , and immune compromised children) diaper dermatitis may become secondarily infected with Candida ablicans. Sometimes severe diaper dermatitis becomes super-infected with bacteria (streptococci or staphylococci).
Demographics
Diaper rashes occur in the diaper-wearing age group (birth to three years of age). Diaper rash occurs in about 10 percent of infants and is most common between the ages of seven and nine months. Some infants seem predisposed to diaper dermatitis. These infants have such sensitive skin that diaper dermatitis is a problem from the first few days of life.
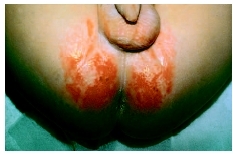
Causes and symptoms
When parents and caretakers do not change the children's diapers often, feces is in contact with skin and irritation develops in the perianal area. Urine left in diapers too long breaks down into ammonia, a chemical that is irritating to infant skin. Ammonia dermatitis of this type is a problem in the second half of the first year of life when the infant is producing a larger quantity of urine.
When the diaper area has prolonged skin contact with wetness the natural oils are stripped away, the outer layer of skin is damaged, and there is increased susceptibility to infection by bacteria or yeast.
Frequently a flat, red rash resulting from chafing of the diaper against tender skin causes friction rash. This rash is not in the skin folds. It may be more definite around the edges of the diaper, at the waist and leg bands. The baby does not seem to experience much discomfort.
Sometimes chemicals in detergents contribute to contact dermatitis . These rashes should clear up as soon as the chemicals are removed. Ignoring the condition may lead to a secondary infection that is more difficult to resolve.
Another infectious cause of diaper rash is impetigo . This bacterial infection is characterized by blisters that ooze and crust.
When to call the doctor
Parents should call the child's healthcare provider for the following reason:
- newborn with rash looks or acts sick or has a fever
- rash looks infected (pimples, blisters, boils, weeping sores, yellow crusts, red streaks)
- rash is not better in three days after treatment for yeast
- rash bright red then peeling off in sheets or raw and bleeding
- rash beyond the diaper area
- rash painful and not responding to home care
Diagnosis
Diagnosis is made by examining the diaper area and taking the history of the onset and duration of the lesions.
The presence of skin lesions means the baby has diaper rash. However, there are several types of rash that may need specific treatment to heal. It is useful to be able to distinguish them by their appearance and causes.
A baby with a rash that does not clear up within two to three days or a rash with blisters or bleeding should receive an evaluation and care from a healthcare professional.
Treatment
Antibiotics are prescribed for rashes caused by bacteria and impetigo. This may be a topical or oral formula, depending on the size of the area involved and the severity of the infection.
Over-the-counter antifungal creams are often used to treat a rash resulting from yeast. If topical treatment is not effective, an oral antifungal is prescribed. Treatment of diaper candida in young infants should include oral drops to treat any candida in the mouth and gut to avoid re-infection.
Mild steroid creams, such as 0.5 to 1 percent hydrocortisone, may be used to treat seborrheic dermatitis and intertrigo. Prescription strength creams are needed for short-term treatment of stubborn cases. Intertrigo can be treated with a combination of hydrocortisone and anti-fungal creams.
Complication
The main complication is secondary infection by yeast or bacteria.
Home care
Good diaper hygiene prevents or clears up many simple cases of diaper rash. Many rashes can be treated as follows:
- Change diapers frequently.
- Keep the area dry and clean. Check the diaper often, every hour if the baby has a rash and change the diaper as soon as it is wet or soiled. Check at least once during the night. Good air circulation is also important for healthy skin. Babies should have some time without wearing a diaper. A cotton pad can protect the bed while the baby is diaper free.
- Frequent and vigorous washing with soap can strip the baby's tender skin of natural protective barriers. Wash gently but thoroughly, including the skin folds. Plain water may be the best cleaning agent when there is a rash. Using warm water in a spray bottle (or give a quick bath) and then lightly pat the skin dry to avoid irritation.
- Instead of cleaning the baby's bottom with a moist wipe or washcloth, hold the diaper area over the sink and let warm water wash over the inflamed skin. Then dry the area using a blow-dryer set on cool. Washing with plain water and drying with air is soothing to sore skin; it speeds healing by decreasing friction on the area. Some wipes contain alcohol or chemicals that can be irritating and only make diaper rash worse.
- Parents can sit the baby in a basin or tub of lukewarm water for several minutes with each diaper change. This helps clean and may also be comforting. Or they can pour warm water from a pitcher or use a squirt bottle. They should not use soap unless there is sticky stool, then a mild liquid soap in a basin of warm water is effective; wash gently and rinse well. Baby oil on a cotton ball can also remove stool from small areas.
- Leave diaper off for a while.
- Do not use airtight rubber pants over the diaper area. Some cloth-like disposable diapers promote better air circulation than plastic-type diapers. If disposable diapers are used, it helps to punch holes in them to let in air.
- Petroleum jelly provides a protective coating, even on sore, redden skin, and is easy to clean. Parents should not use talcum powder because of the risk of pneumonia . However, cornstarch reduces friction and may prevent future rashes.
Nutrition
What the baby eats can make a difference in stool frequency and acidity. Typically, breast-fed babies have fewer problems with rashes. When adding a new food to the diet, the baby should be watched closely to see whether rashes appear around the baby's mouth or anus. If they do, the new food should be avoided temporarily.
Babies who are taking antibiotics are more likely to get rashes because of yeast. To help bring the good bacterial counts back to normal, Lactobacillus bifidus can be added to the diet. It is available in powder form from most health food stores.
Herbal treatment
Some herbal preparations can be useful for diaper rash. Calendula reduces inflammation, tightens tissues, and disinfects. It is recommended for seborrheic dermatitis as well as for general inflammation of the skin. The ointment should be applied at each diaper change. Chickweed ointment can also sooth irritated skin when it is applied once or twice daily.
Prognosis
With proper treatment these rashes are usually better in three days if there is no underlying health problem or skin disease. If the rash does not improve with treatment then the child probably has a yeast infection. In that case, the rash becomes bright red and raw, covers a large area, and is surrounded by red dots. For yeast infection, the child needs a special cream.
Prevention
Changing the diaper immediately and good cleaning are the best action a parent can take to prevent diaper rash. Diaper rashes occur equally with cloth diapers and disposable diapers. Some children will get a rash from certain brands of disposable diapers or from sensitivity to some soaps used in cloth diapers. If cloth diapers are used, always wash them separate from other clothing and add bleach to the soap. After washing, the diapers should be rinsed thoroughly.
Parental concerns
Diapering. There are two choices, cloth or disposable. Parents need to decide what works best for their baby and lifestyle.
In the event of suspected yeast, a tablespoon of cider vinegar in a cup of warm water can serve as a diaper area wash. This is diluted enough that it should not burn, but acidifies the skin pH enough to hamper the yeast growth.
Barrier ointments can be valuable to treat rashes. Those that contain zinc oxide are especially effective. These creams and ointments protect already irritated skin. Cornstarch powder is soothing to rashes that are moist, such as impetigo.
KEY TERMS
Dermatitis —Inflammation of the skin.
Diaper dermatitis (diaper rash) —An inflammatory reaction to irritants in the diaper area.
Impetigo —A bacterial infection of the skin characterized by skin blistering.
Lactobacillus bifidus —A property of breast milk that interferes with the growth of pathogenic bacteria in the gastrointestinal tracts of babies, reducing the incidence of diarrhea. Lactobacillus bifidus can be added to infant formulas to help control diarrhea.
Resources
BOOKS
Middlemiss, Prisca. What's That Rash?: How to Identify and Treat Childhood Rashes. London: Hamlyn, 2002.
WEB SITES
Kazzi, Amin, and Khoa Nguyen. "Pediatrics: Diaper Rash." eMedicine.com , November 1, 2004. Available online at http://www.emedicine.com/emerg/topic374.htm (accessed December 15, 2004).
Aliene S. Linwood, RN, DPA, FACHE