Circumcision
Definition
The surgical removal of the foreskin of the penis in a male or the prepuce of a clitoris in a female.
Purpose
In the United States, circumcision in infant boys is performed for social, medical, cultural, or religious reasons. Once a routine operation urged by pediatricians and obstetricians for newborns in the middle of the twentieth century, circumcision has become an elective option that parents make for their sons on an individual basis. Families who practice Judaism or Islam may select to have their sons circumcised as a religious practice. Others may elect circumcision for medical reasons.
Female circumcision (also known as female genital mutilation) is usually performed for cultural and social reasons by family members and others who are not members of the medical profession, with no anesthesia. Not only is the prepuce of the clitoris removed but often the vaginal opening is sewn to make it smaller. This practice is supposed to ensure the virginity of a bride on her wedding day. It also prevents the woman from achieving sexual pleasure during coitus. Female circumcision is illegal in most countries of the world. It is considered by most people to be a human rights violation.
Though the incidence of male circumcision has decreased from 90 percent in 1979 to 60 percent in 2002, it is still the most common surgical procedure in the United States. Circumcision rates are much lower for the rest of the industrialized world. In Britain, it is only performed for religious practices or to correct a specific medical condition of the penis.
Parents may choose circumcision because they believe the surgery protects against infections of the urinary tract and the foreskin, prevents cancer , lowers the risk of getting sexually transmitted diseases , and prevents phimosis (a tightening of the foreskin that may close the opening of the penis). Though studies indicate that uncircumcised boys under the age of five are 20 times more likely than circumcised boys to have urinary tract infections (UTIs), the rate of incidence of UTIs is quite low. There are also indications that circumcised men are less likely to suffer from penile cancer, inflammation of the penis, or have many sexually transmitted diseases. Here again, the rate of incidence is low. Good hygiene usually prevents most infections of the penis. Phimosis and penile cancer are very rare, even in men who have not been circumcised. Education and good safe-sex practices can prevent sexually transmitted diseases in ways that a surgical procedure cannot because these are diseases acquired through risky behaviors.
With these factors in mind, the American Academy of Pediatrics issued a policy pronouncement that states although there is existing scientific evidence that support the medical benefits of circumcision, the benefits are not strong enough to recommended circumcision as a routine practice.
Description
The foreskin of the penis safeguards the sensitivity of the glans and shields it from irritation by urine, feces, and foreign materials. It also protects the urinary opening against infection and accidental injury.
Despite a long-standing belief that infants do not experience serious pain from circumcision, most authorities in the early 2000s believe that some form of local anesthesia is necessary. The physician injects local anesthesia at the base of the penis or under the skin around the penis (subcutaneous ring block). Both anesthetics block key nerves. EMLA cream, a topical formula of several anesthetics, can also be used.
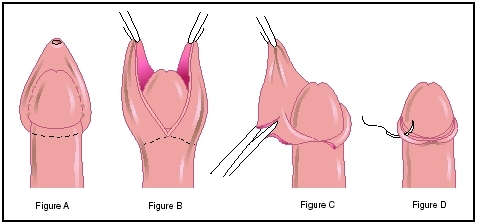
In circumcision of infant boys, the foreskin is pulled tightly into a specially designed clamp. Pressure is applied and the foreskin pulls away from the broadened tip of the penis. Pressure from the clamp stops bleeding from blood vessels that supplied the foreskin. In older boys or adults, an incision is made around the base of the foreskin, the foreskin is pulled back, and then it is cut away from the tip of the penis. Stitches are usually used to close the skin edges.
After circumcision, the wound should be washed daily. An antibiotic ointment or petroleum jelly may be applied to the site. If there is an incision, a wound dressing will be present and should be changed each time the diaper is changed. Sometimes a plastic ring is used instead of a bandage. The ring usually falls off in five to eight days. The penis heals in seven to 10 days.
Infants who undergo circumcision may be fussy for some hours afterward, so parents should be prepared for crying, feeding problems, and sleep problems. Generally these go away within a day. In older boys, the penis may be painful, but the pain goes away gradually. A topical anesthetic ointment or spray may be used to relieve this temporary discomfort. There may also be a bruise on the penis, which typically goes away with no particular attention.
The clitoral prepuce of infant girls is drawn up and away from the body before being removed. In this procedure, the clitoris is also frequently removed. The vaginal opening may be partially closed. Healing is slower in girls than for boys. Most female circumcisions are performed under unhygienic conditions using primitive, homemade implement such as rusty razor blades and thorns. Infections are common.
Risks
Complications following newborn circumcision appear in one out of every 500 procedures. Most complications are minor. Bleeding occurs in half of the complications and is usually easy to control. Infections are rare and present with fever and signs of inflammation. Uneven healing of skin may lead to laterally curving erections in adulthood.
There may be injuries to the body of the penis that may be difficult to repair. In 2000, there were reports that the surgical clamps used in circumcision were at fault in over 100 injuries reported between July 1996 and January 2000. In nearly all cases, the clamps were assumed to be in working order but had been repaired with replacement parts that were not of the manufacturer's specifications. Physicians were urged to inspect the clamps before use and ensure that their dimensions fit the infant's body parts.
Circumcised girls have a high incidence of infertility and sexual dysfunction as adults. Most experience infections immediately after the procedure.
Normal results
Among boys who are circumcised, most have no penile, urologic, or sexual dysfunction as adults. A majority of girls who are circumcised experience urologic, reproductive, and sexual dysfunction as adults.
KEY TERMS
Foreskin —A covering fold of skin over the tip of the penis.
Glans penis —The cone-shaped tip of the penis.
Hernia —A rupture in the wall of a body cavity, through which an organ may protrude.
Hydrocele —A collection of fluid between two layers of tissue surrounding the testicle; the most common cause of painless scrotal swelling.
Hypospadias —A congenital abnormality of the penis in which the urethral opening is located on the underside of the penis rather than at its tip.
Phimosis —A tightening of the foreskin that may close the opening of the penis.
Prepuce —A fold of skin, such as the foreskin of the penis or the skin that surrounds the clitoris.
Parental concerns
The only medical justification for male circumcision is to correct a health problem or condition. There are no medical justifications for female circumcision. The only other justification for male or female circumcision is religious or cultural. Leaders of the vast majority of religions throughout the world condemn any form of female circumcision.
Resources
BOOKS
Darby, Robert. A Surgical Temptation: The Demonization of the Foreskin and the Rise of Circumcision in Britain. Chicago: University of Chicago Press, 2005.
Elder, Jack S. "Anomalies of the Penis and Urethra." In Nelson Textbook of Pediatrics , 17th ed. Edited by Richard E. Behrman, et al. Philadelphia: Saunders, 2003, pp. 1812–6.
Fleiss, Paul M., and Frederick Hodges. What Your Doctor May Not Tell You about Circumcision: Untold Facts on America's Most Widely Performed—and Most Unnecessary Surgery. New York: Warner Books, 2002.
Gollaher, David L. Circumcision: A History of the World's Most Controversial Surgery. New York: Basic Books, 2000.
Lewis, Joseph, et al. In the Name of Humanity: Speaking Out against Circumcision. San Diego, CA: Book Tree, 2003.
PERIODICALS
Adelman, W. P., and A. Joffe. "Controversies in male adolescent health: varicocele, circumcision, and testicular self-examination." Current Opinions in Pediatrics 16, no. 4 (2004): 363–7.
Campbell, C. C. "Care of women with female circumcision." Journal of Midwifery and Women's Health 49, no. 4 (2004): 364–5.
Essen, B., and S. Johnsdotter. "Female genital mutilation in the West: traditional circumcision versus genital cosmetic surgery." Acta Obstetrics and Gynecology of Scandinavia 83, no. 7 (2004): 611–3.
Hiss, J., A. Horowitz, and T. Kahana. "Fatal hemorrhage following male ritual circumcision." Journal of Clinical Forensic Medicine 7, no. 1 (2000): 32–4.
ORGANIZATIONS
American Academy of Family Physicians. 11400 Tomahawk Creek Parkway, Leawood, KS 66211–2672. Web site: http://www.aafp.org/.
American Academy of Pediatrics. 141 Northwest Point Boulevard, Elk Grove Village, IL 60007–1098. Web site: http://www.aap.org/.
American College of Surgeons. 633 North St. Clair Street, Chicago, IL 60611–32311. Web site: http://www.facs.org/.
American Medical Association. 515 N. State Street, Chicago, IL 60610. Web site: http://www.ama-assn.org/.
American Urological Association. 1120 North Charles Street, Baltimore, MD 21201. Web site: http://www.auanet.org/index_hi.cfm.
WEB SITES
"Circumcision." Circumcision Information Resource Pages. Available online at http://www.cirp.org/ (accessed November 2, 2004).
"Circumcision." Available online at Circumcision Resource Center. Available online at http://www.circumcision.org/ (accessed November 2, 2004).
"Circumcision." Mothers Against Circumcision. Available online at http://www.mothersagainstcirc.org (accessed November 2, 2004).
"Doctors Opposing Circumcision." University of Washington. Available online at http://faculty.washington.edu/gcd/DOC/ (accessed November 2, 2004).
L. Fleming Fallon Jr., MD, DrPH
Do add more like this kind..
Should your explanation include that a male foreskin is a body part and should be left intact unless medical need arises? Hygeine and condom use seem like better methods to control UTI and STD risks rather than removal of a body part.
Is there a healthy body part that is frequently removed other then the foreskin of infants to prevent cancer, STDs and infection? Medical terminology should be presented without our own cultural biases.