Appendicitis
Definition
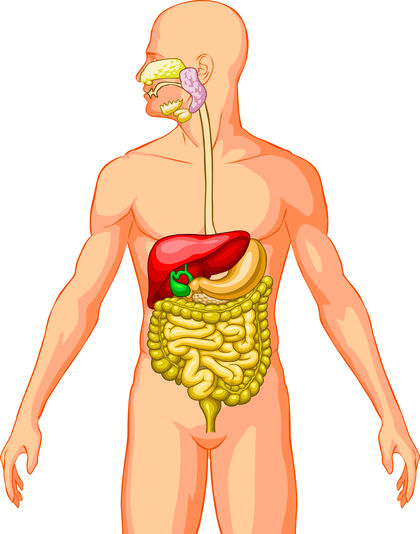
Appendicitis is an inflammation of the appendix, which is the small, finger-shaped pouch attached to the beginning of the large intestine on the lower-right side of the abdomen. Appendicitis is a medical emergency, and if left untreated, the appendix may rupture and cause a potentially fatal infection.
Description
In children, appendicitis is the most common abdominal medical emergency and most common pediatric emergency surgical procedure. Although the appendix has no known function, it can become inflamed and diseased. This condition, called appendicitis, can rapidly evolve into a life-threatening or fatal infection of the abdominal cavity (peritonitis) if not treated immediately. Appendicitis usually involves emergency consultation with a physician and evaluation in a hospital emergency department.
Demographics
Appendicitis is the most common abdominal emergency found in children and young adults. One person in 15 develops appendicitis in his or her lifetime. The incidence is highest among males aged 10 to 14, and among females aged 15 to 19. More males than females develop appendicitis between puberty and age 25. It is rare in infants and children under the age of two. In the United States, appendicitis occurs in four out of 1,000 children.
Causes and symptoms
Appendicitis is usually caused by a blockage of the inside of the appendix, which is called the lumen. Most often, the lumen is blocked by fecal material. Lymphoid tissue, which is present in mucosal lining of the appendix and intestines to help fight bacterial and viral infections, can swell and lead to obstruction of the appendix. This condition, called lymphoid hyperplasia, may also be associated with a variety of inflammatory and infectious diseases, such as Crohn's disease, gastroenteritis , respiratory infections, mononucleosis, and measles . Appendicitis can also be caused by foreign bodies (e.g., intrauterine device or something swallowed), traumatic abdominal injury, or tumors. In addition, genetics may play a role in appendicitis; some children may inherit genes that make them more susceptible to blockage of the appendiceal lumen. Having cystic fibrosis also increases a child's risk for appendicitis.
Blockage of the appendix then causes inflammation, increased pressure, and restricted blood flow, leading to abdominal pain and tenderness in the right lower quadrant of the abdomen. If the appendix is not removed, bacteria and inflammation within the appendix rapidly expand, the wall of the appendix stretches, and perforation can occur. Once the appendix is perforated, bacteria-filled fluid is released into the abdominal cavity and peritonitis then develops. Perforation is more common in younger children. Perforation can occur as soon as 48 to 72 hours after symptoms first begin and can become life-threatening.
Classic symptoms of appendicitis include the following:
- abdominal pain, first around the navel then moving to the lower right quadrant of the abdomen
- nausea
- vomiting
- loss of appetite
- diarrhea, constipation , and/or inability to pass gas
- fever beginning after other symptoms
- abdominal swelling and tenderness
Other possible symptoms are pain on urination, inability to urinate, or frequent urge to urinate if the swollen appendix is near the urinary tract and bladder. When perforation occurs, abdominal pain becomes more intense and involves the whole abdominal area, and fever may be very high.
Symptoms of appendicitis vary, and not every child will have all the symptoms. In children younger than age two years, the most common symptoms are vomiting and a bloated or swollen abdomen. Toddlers with appendicitis may have difficulty eating and may seem very tired. Children may have constipation, but may also have small stools that contain mucus. Although infants and children younger than two years may also have abdominal pain and other symptoms, they are too young to effectively communicate their symptoms to adults, who may then miss the symptoms of appendicitis.
When to call the doctor
Appendicitis is a medical emergency. A doctor should be called immediately if appendicitis is suspected so that children can receive prompt medical treatment before perforation occurs. Parents who suspect that their child has appendicitis should not give the child any pain medication because it may interfere with the results of a doctor's physical examination for appendicitis. In addition, parents should not give their child anything to eat or drink in case surgery is required immediately.
Symptoms in combination that require a doctor's immediate attention include significant abdominal pain, fever, diarrhea, nausea and vomiting , swollen or bloated abdomen, and loss of appetite. If abdominal pain begins before nausea and vomiting, rather than after, appendicitis rather than intestinal infection is more likely.
Diagnosis
Appendicitis is diagnosed by physical examination, laboratory tests, and imaging tests. During a physical examination, the doctor palpates the abdomen to find tender and painful spots. A physical examination can also include a rectal examination, examination of the genitals in boys, and a gynecologic examination in girls, because other conditions, such as testicular torsion and ectopic pregnancy may have symptoms similar to appendicitis. Laboratory tests involve an analysis of white blood cell count to determine whether infection is present, urinalysis to rule out urinary tract or kidney infection, and other tests, such as pregnancy and liver function tests, to rule out other causes of abdominal pain. Imaging tests can include abdominal x rays, ultrasound, and computed tomography (CT).
In 2004, a new imaging technique that uses nuclear medicine imaging and an injection of an imaging agent called NeutroSpec was introduced for the diagnosis of appendicitis.
Abdominal pain is a common complaint in children, and making a timely diagnosis of appendicitis before perforation is often difficult. Up to 30 percent of children with appendicitis are misdiagnosed, even by experienced physicians. In infants, diagnosis is often not possible and not made until after perforation. Appendicitis is most often misdiagnosed as gastroenteritis or respiratory infection.
Treatment
Appendicitis is treated by immediate surgery to remove the appendix, called an appendectomy. Appendectomy is the most common emergency surgery performed by pediatric surgeons. In an open appendectomy, the appendix is removed through a standard abdominal incision. In laparoscopic appendectomy, surgeons insert a small scope through tiny abdominal incisions to remove the appendix. A laparoscopic appendectomy results in less postoperative pain and fewer surgical incision infections. However, the procedure is longer and requires specialized surgical experience in operating on pediatric patients. In female teen patients, laparascopy has the added benefit of being able to diagnose and treat gynecologic conditions and ectopic pregnancy during the appendectomy if the appendix is found to be normal.
Preoperative antibiotics are given to children with suspected appendicitis and stopped after surgery if there is no perforation. Antibiotic treatment kills bacteria, and stronger and longer courses of antibiotics are required if peritonitis occurs.
If the appendix is removed before perforation occurs, the hospital stay is usually two to three days. A child with a perforated appendix and peritonitis must remain in the hospital up to a week.
Prognosis
Appendicitis is usually treated successfully by appendectomy, and unless there are complications, children should recover without further problems. The mortality rate in cases without complications is less than 0.1 percent. Perforated and ruptured appendix, as well as peritonitis, occur at higher rates among children. When the appendix has ruptured or a severe infection has developed, the likelihood for developing complications is higher, and recovery is longer. Peritonitis is a life-threatening condition, and death occurs in about 1 percent of cases.
Prevention
In general, appendicitis cannot be prevented. The incidence of appendicitis is lower in cultures where people eat more daily dietary fiber, which is thought to decrease the viscosity of feces, decrease bowel transit time, and discourage formation of fecaliths, which predispose individuals to obstructions within the appendix.
Parental concerns
Because the appendix is more likely to perforate in children than adults, parents should not hesitate to call the doctor if their child develops symptoms that may indicate appendicitis. Parents should feel free to ask their doctor and other medical staff questions about any medical tests or treatments their child receives.
KEY TERMS
Appendectomy —Surgical removal of the appendix.
Appendix —The worm-shaped pouch attached to the cecum, the beginning of the large intestine.
Computed tomography (CT) —An imaging technique in which cross-sectional x rays of the body are compiled to create a three-dimensional image of the body's internal structures; also called computed axial tomography.
Ectopic pregnancy —A pregnancy that develops outside of the mother's uterus, such as in the fallopian tube. Ectopic pregnancies often cause severe pain in the lower abdomen and are potentially life-threatening because of the massive blood loss that may occur as the developing embryo/fetus ruptures and damages the tissues in which it has implanted.
Laparoscopy —A surgical procedure in which a small incision is made, usually in the navel, through which a viewing tube (laparoscope) is inserted. This allows the doctor to examine abdominal and pelvic organs. Other small incisions can be mad to insert instruments to perform procedures. Laparoscopy is done to diagnose conditions or to perform certain types of surgeries.
Peritonitis —Inflammation of the peritoneum. It is most often due to bacterial infection, but can also be caused by a chemical irritant (such as spillage of acid from the stomach or bile from the gall bladder).
Testicular torsion —A condition involving the twisting of the spermatic cord inside the testicle that shuts off its blood supply and can seriously damage the testicle.
Ultrasonography —A medical test in which sound waves are directed against internal structures in the body. As sound waves bounce off the internal structure, they create an image on a video screen. Ultrasonography is often used to diagnose fetal abnormalities, gallstones, heart defects, and tumors. Also called ultrasound imaging.
Resources
BOOKS
Majumdar, P. C. Appendicitis. New Delhi, India: B. Jain, 2003.
Tilden, J. H. Appendicitis: The Etiology, Hygienic, and Dietetic Treatment. Pahrump, NV: Library of New Atlantis, 2003.
Harvard Medical School. Medical Tests: A Practical Guide to Common Tests. Boston, MA: Harvard Health Publications, 2004.
PERIODICALS
Kosloske, A. M., et al. "The Diagnosis of Appendicitis in Children: Outcomes of a Strategy Based on Pediatric Surgical Evaluation." Pediatrics 113 (January 2004): 29–34.
McCullough, M. "Targeting Appendicitis: A New Tool Offers Wider Promise." Philadelphia Inquirer (July 7, 2004).
Zitsman, J. L. "Current Concepts in Minimal Access Surgery for Children." Pediatrics 111 (June 2003): 1239–52.
ORGANIZATIONS
American College of Emergency Physicians. Web site: http://www.acep.org.
American College of Radiology. Web site: http://www.acr.org.
WEB SITES
"Appendicitis." Available online at http://kidshealth.org/parent/infections/stomach/appendicitis.html (accessed October 24, 2004).
"Appendicitis." National Digestive Diseases Information Clearinghouse. Available online at http://digestive.niddk.nih.gov/ddiseases/pubs/appendicitis/ (accessed October 24, 2004).
Trevino, M. "CT for Appendicitis Diagnosis in Children Gains Popularity." Available online at http://www.dimag.com/dinews/2003050901.shtml (accessed October 24, 2004).
Tucker, J. "Pediatrics: Appendicitis." Emedicine. Available online at http://www.emedicine.com/emerg/topic361.htm (accessed October 24, 2004).
Jennifer E. Sisk, M.A.