Polio vaccine
Definition
The poliomyelitis ( polio ) vaccine protects against poliovirus infections. The vaccine helps the body produce antibodies (protective substances) that will prevent an individual from contracting polio. There are two forms of the vaccine that can be given; the one preferred is the inactivated poliovirus vaccine (IPV). IPV is preferred because it contains the inactivated or dead virus, which is considered safer for administration. The Sabin oral polio vaccine was made with a live but weakened virus, which gives the advantage of passive immunity for large groups (i.e. because it is easily passed on through the oral fecal route in households, schoolrooms, etc., even if only a portion of the community is immunized, everyone eventually develops immunity). The Sabin oral polio vaccine has the disadvantage of causing polio-like symptoms in some immune compromised hosts. Since 2000, the live virus vaccine is rarely used in the United States, but it is still being used in other countries.
Description
The purpose of any vaccine is to prevent disease. Mass immunizations in the United States have served to eradicate polio in the Americas. In 1988, the World Health Organization embarked upon a mission to eradicate polio by the year 2000. The intent was to immunize the world's children by methodically establishing sites where the masses could be reached. The mandate was to eradicate the virus by 2005. Most of the remaining virus can be found on the Indian subcontinent and Nigeria. Attempts to immunize children in Indian have met with good results, but Nigeria halted their immunization sites due to rumors that Western donors had tampered with the vaccine to spread HIV and cause sterility in Muslim males. Following a ban on the vaccine that lasted nearly one year, the virus spread across Nigeria to 10 African countries that were previously polio-free. The Muslim leaders in Nigeria lifted the ban in summer 2004. Immunization from the IPV triggers an excellent immune response and long-lasting immunity to all three poliovirus types.
General use
The inactivated poliovirus vaccine is injected into a muscle or under the skin and is usually given by a health care professional in a hospital, clinic, or provider's office. The use of this vaccine must be officially recorded. Federal law requires that the vaccine manufacturer's name, the lot number of the vaccine, the name, address, and phone number of the person giving the vaccine, and the date of vaccine administration be recorded in a permanent medical record. For children, the vaccine is usually started at two months of age and given again at four months of age. The next dose should be given between six and 18 months of age with a final booster dose at age four to six years, for a total of four doses. Serious reactions to the inactivated poliovirus vaccine are rare in small children. It is necessary to receive all doses of the vaccine and there is no generic vaccine available.
Precautions
Individuals with an immune deficiency disease need to be counseled before taking the vaccine, and anyone with allergic reactions to prior vaccines and preservatives should be cautious. A provider may want to delay giving a child a dose of IPV or may not give it at all if the child has a known severe allergy to the antibiotics neomycin, streptomycin, or polymyxin B. A child who had a life-threatening reaction to a previous IPV should not receive another one.
There is no preparation necessary for the vaccine; however, if an individual is ill on the scheduled date, it is essential to make arrangements for a follow-up appointment as no dose can be missed.
Side effects
Children receiving the inactivated poliovirus vaccine should be carefully observed for 24–72 hours after receiving the injection. If any serious side effects occur, the healthcare provider or an emergency service provider should be called immediately. For problems that may occur following the vaccine, parents are asked to call the vaccine adverse event reporting system toll-free at (800) 822–7967 to report them. The health care professional may administer a dose of a non-aspirin pain/fever reliever at the time of the vaccine and advise giving the medicine every four to six hours for 24 hours after the vaccine. This may serve to reduce pain and fever associated with the vaccine.
Side effects that usually do not require immediate medical attention, unless they persist and are bothersome, include:
- fussiness
- decreased appetite
- low-grade fever (102°F [39° C] or less)
- pain, tenderness, redness, swelling, or a "knot" at the injection site
- fatigue
- vomiting
Side effects that should be reported as soon as possible are:
- limp, pale, or less alert child
- difficulty breathing, shortness of breath, or wheezing
-
difficulty swallowing
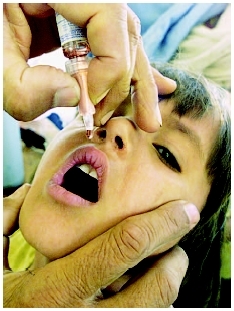 Oral polio vaccines are no longer recommended for use in the United States, but are still used in many parts of the world.(© Reuters/Corbis)
Oral polio vaccines are no longer recommended for use in the United States, but are still used in many parts of the world.(© Reuters/Corbis) - high fever (103°F [39.4°C] or more)
- inconsolable crying for three hours or more
- seizures (convulsions)
- severe skin rash, hives , or itching
- swelling of eyes or face
- unusual sleepiness
Interactions
Before administering the vaccine, the healthcare provider should be informed as to whether the recipient has any of the following conditions:
- an immune deficiency (natural or due to cancer chemotherapy radiation, steroid therapy, or HIV infection)
- fever or infection
- an unusual reaction to this poliovirus vaccine, oral poliovirus vaccine, other medicines, foods, dyes, or preservatives
- pregnant or trying to get pregnant
- breastfeeding
Prevention
While it is important to mention these items to the physician, they are not necessarily contraindications for the vaccine. The provider also needs to know what medicines an individual is taking, including non-prescription medicines, nutritional supplements, herbal products, tobacco, and whether or not he or she is a user of illegal drugs or a frequent user of drinks with caffeine or alcohol. Any of these may affect the way the vaccine works.
Risks
There have been no adverse effects from IPV reported to date. However, IPV induces only little immunity in the intestinal tract. If an individual is infected with the wild-type poliovirus, the virus can multiply in the intestines and be shed in stools, ultimately heightening the risk of viral circulation within the community. This scenario is unlikely in the United States.
Parental concerns
Parents need to be aware of any existing allergies in their families that might cause a reaction from vaccines and their preservatives, and they need to be observant of a child for the first 24–72 hours after receiving the vaccine. Traveling to other parts of the world may necessitate a booster vaccine if the polio virus is known to be present in that vicinity.
KEY TERMS
World Health Organization (WHO) —An international organization within the United Nations system that is concerned with world health and welfare.
See also Polio .
Resources
BOOKS
2004 Childhood and Adolescent Immunization Schedule. Atlanta: GA, Centers for Disease Control and Prevention, 2004. http://www.cdc.gov/nip/recs/childschedule.htm#Printable
PERIODICALS
Osterrieth, Paul. "Oral polio vaccine: fact vs. fiction." Vaccine 22 (2004): 1831–35. http://www.elsevier.com/locate/vaccine
ORGANIZATIONS
March of Dimes Birth Defects Foundation. National Office, 1275 Mamaroneck Avenue, White Plains, NY 10605. http://www.modimes.org/
WEB SITES
"Polio Vaccine." http://familydoctor.org/x1998.xml.
World Health Organization. Global Polio Eradication Progress 2000. http://www.polioeradication.org/
Linda K. Bennington, MSN, CNS
Comment about this article, ask questions, or add new information about this topic: