Warts
Definition
Warts are small, benign growths caused by a viral infection of the skin or mucous membrane. The virus infects the surface layer. The viruses that cause warts are members of the human papilloma virus (HPV) family. Warts are not cancerous, but some strains of HPV, usually not associated with warts, have been linked with cancer formation. Warts are contagious from person to person and from one area of the body to another on the same person.
Description
There are approximately 60 types of HPV that cause warts, each preferring a specific bodily location. For instance, some types of HPV cause warts to grow on the skin, others cause them to grow inside the mouth, while still others cause them to grow on the genital and rectal areas. However, most can be active anywhere on the body. The virus enters through the skin and produces new warts after an incubation period of one to eight months. Warts are usually skin-colored and feel rough to the touch, but they also can be dark, flat, and smooth.
Warts are passed from person to person, directly and indirectly. Some people are continually susceptible to warts, while others are more resistant to HPV and seldom get them. The virus takes hold more readily when the skin has been damaged in some way, which may explain why children who bite their nails tend to have warts located on their fingers. People who take a medication to suppress their immune system or are on long-term steroid use are also prone to a wart virus infection. This tendency is seen in people with AIDS .
Demographics
Particularly common among children, young adults, and women, warts are a problem for 7–10 percent of the population.
Causes and symptoms
The more common types of warts include the following:
- common hand warts
- foot warts
- flat warts
- genital warts
Hand warts
Common hand warts grow around the nails, on the fingers, and on the backs of hands. They appear more frequently where skin is broken, such as in areas where fingernails are bitten or hangnails are picked.
Foot warts
Foot warts are called plantar warts because the word plantar is the medical term for the sole of the foot, the area where the wart usually appears as a single lesion or as a cluster. Plantar warts, however, do not stick up above the surface like common warts. The ball of the foot, the heel, and the plantar part of the toes are the most likely locations for the warts because the skin in those areas is subject to the most weight, pressure, and irritation, making a small break or crack more likely.
Plantar warts are familiar to all ages groups, appearing frequently in children between the ages of 12 and 16. Adolescents often come into contact with a wart virus in a locker room, swimming pool area, or by walking barefooted on dirty surfaces. The blood vessels feeding them are the black dots that are visible on the wart. If left untreated, these warts can grow to an inch or more in circumference and spread into clusters of several warts. They are known to be very painful at times, the pain
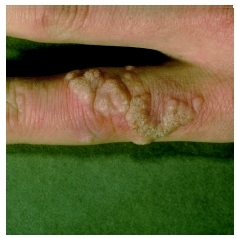
Flat warts
Flat warts tend to grow in great numbers and are smaller and smoother than other warts. They can erupt anywhere, appearing more frequently on the legs of women, the faces of children, and on the areas of the face that are shaved by young adult males.
Genital warts
Genital warts, also called condyloma acuminata or venereal warts, are one of the most common forms of sexually transmitted disease (STD) in this country. Most experts contend that they are contracted by sexual contact with an infected person who carries HPV and are more contagious than other warts. It is estimated that two-thirds of the people who have sexual contact with a partner with genital warts will develop the disease within three months of contact. As a result, about 1 million new cases of genital warts are diagnosed in the United States each year.
Genital warts tend to be small flat bumps but they may be thin and tall. They are usually soft and not scaly like other warts. In women, genital warts appear on the genitalia, within the vagina, on the cervix, and around the anus or within the rectum. In men, genital warts usually appear on the tip of the penis but may also be found on the scrotum or around the anus. Genital warts can also develop in the mouth of a person who has had oral sexual contact with an infected person.
When to call the doctor
Individuals who notice warts in their genital area should see a doctor. A physician should be consulted for warts that bleed, are particularly painful, or that do not disappear after six to nine months.
Diagnosis
A physician may be able to diagnose warts with a simple examination. If the warts are small, the doctor may put a vinegar-like liquid on the skin, which makes the warts turn white and easier to see, and then use a magnifying glass to look for them.
Treatment
Most people attempt to treat warts themselves. Professional treatment is usually sought after self-treatment has been unsuccessful.
Home/self treatment
Many of the nonprescription wart remedies available at drug stores will remove simple warts from hands and fingers. These medications may be lotions, ointments, or plasters and work by chemically removing the skin that was affected by the wart virus. The chemicals are strong, however, and should be used with care since they can remove healthy as well as infected skin. These solutions should be avoided by diabetics and those with cardiovascular or other circulatory disorders whose skin may be insensitive and not appreciate irritation.
Flat warts are best treated with topical retinoides (retinoic acid) or a gel containing salicylic acid. The acid does not actually kill the wart virus, but waterlogs the skin so that the surface layer, with the virus, peels off. These products can take up to three months of treatment depending on the size and depth of the wart. Patches are also good to use. Rather than applying drops, a small pad is placed on the wart and left for 48 hours and then replaced with a new one. The patch usually contains a higher concentration of salicylic acid and may irritate the surrounding skin. If this occurs, people should switch to a gel or stop medication for a period. To help the healing process for flat facial warts, men should shave with an electric shaver or temporarily grow a beard. Women with flat warts on areas that are shaved should use other methods to remove hair such as depilatory cream or wax.
Professional treatment
Physicians should be consulted if there are no signs of progress after a month of self treatment. Doctors have many ways of removing warts, including using stronger topically applied chemicals than those available in pharmacies. Some of these solutions include podofilox, topical podophyllum, and trichloracetic acid (TCA). Some burning and discomfort for one or more days following treatment can be expected. Although these chemicals are effective, they may not completely destroy all warts. A second method of removal is freezing or cryosurgery on the wart using liquid nitrogen. Cryotherapy is relatively inexpensive, does not require anesthesia, and usually does not result in scarring. Although temporarily uncomfortable, it provides an effective and safe way to deliver freezing temperatures to a particular area on the skin, and healing is usually quick. Physicians may also choose to burn the wart with liquid nitrogen or numb the skin and then scrape off the wart. Another removal process is electrocautery (electric burning), destroying the wart by burning it with an electric needle. Laser surgery is also an option for removing warts.
Genital warts are the most difficult to treat. They can be removed, but the viral infection itself cannot be cured. Often, because the warts are so small, more than one treatment may be needed. The virus continues to live in the deeper skin, which is why warts often return after they have been removed. Strong chemicals may be applied as well as surgical excision with or without electrocautery. This therapy requires a small operative procedure and a local anesthetic. Laser therapy, although more expensive, is often used for treating venereal warts that are more extensive. The use of lasers, which vaporize the lesion, can theoretically transmit the HPV. It is not at all clear, however, if this occurs.
There is no single recommended method for eliminating plantar warts. If detected early, cryotherapy is usually enough. However, they can be very resilient, requiring repeated treatment over several months. Treatment ranges from the conservative approach of applying chemical solutions to the more aggressive option of surgery. Persons with diabetes or vascular disease are usually treated with the more conservative methods.
Alternative treatment
There are a variety of alternative approaches to the treatment of warts. The following suggestions apply to common warts and plantar warts. They are not recommended for genital or cervical warts. Since genital and cervical warts are transmitted sexually, they should be treated by a physician.
For the treatment of common or plantar warts, practitioners may recommend the following remedies:
- Apply a paste made of vitamin C powder to the wart for one to two weeks.
- Place a crushed or sliced garlic clove over the wart for seven consecutive nights while sleeping.
- Soak the wart in water, put cross-hatches over it with a sterile needle, and apply drops of thuja ( Thuja occidentalis ) tincture onto the wart. Repeat the crosshatching and tincture application until the wart is saturated with the tincture. Repeat several times each day for one to two weeks. (A tincture is an herbal extract made with alcohol.)
- Tape a piece of banana peel, smooth side down, over the wart and leave it on overnight. Repeat nightly for one to two weeks.
Prognosis
Even though genital warts may be removed, the virus itself continues to live. The HPV can cause tissue changes in the cervix of women with cervical infection. The general recommendation for women who have a history of genital warts is to see their doctors every six months for Pap smears to monitor any changes that may occur.
For plantar warts, the treatment goal is to destroy the wart and its virus without causing much damage to healthy skin. It is not unusual for treatment to cause pain until the foot heals because of the weight put on the foot.
Prevention
Plantar warts can be prevented by wearing shoes, changing shoes daily, keeping feet clean and dry, and not ignoring skin growths and changes in the skin. Genital warts can be prevented by using condoms and avoiding unprotected sex. Barrier protection will not, however, prevent the spread of wart-causing HPV to uncovered areas such as the pubis and upper thighs.
Nutritional concerns
Because warts are caused by a virus, general immune system support can be effective in helping to keep warts from coming back after treatment or to keep them from multiplying or growing. Eating a well balanced diet high in sources of vitamins A, C, and E can help strengthen the immune system. Avoiding stress, which is believed to compromise the immune system, may also be helpful.
Parental concerns
Parents can help to prevent plantar warts by urging their children to wear shoes, change their shoes daily, and keep their feet clean and dry. Parents should also pay attention to growths and other changes in their child's skin. Instructing children in condom usage is a personal, parental decision. However, parents should tell their children that genital warts can be prevented by using condoms and avoiding unprotected sex. Barrier protection will not, however, prevent the spread of wart-causing HPV to uncovered areas such as the pubis and upper thighs.
KEY TERMS
Condyloma acuminata —Another term for a genital wart.
Cryotherapy —The use of a very low-temperature probe to freeze and thereby destroy tissue. Cryotherapy is used in the treatment skin lesions, Parkinson's disease, some cancers, retinal detachment, and cataracts. Also called cryosurgery.
Endometritis —Inflammation of the endometrium or mucous membrane of the uterus.
Epidermis —The outermost layer of the human skin.
Human papilloma virus (HPV) —A virus that causes common warts of the hands and feet, as well as lesions in the genital and vaginal area. More than 50 types of HPV have been identified, some of which are linked to cancerous and precancerous conditions, including cancer of the cervix.
Retinoic acid —Vitamin A 1 acid which is used topically to treat acne.
Salicylic acid —An agent prescribed to treat a variety of skin disorders, such as acne, dandruff, psoriasis, seborrheic dermatitis, calluses, corns, and warts.
Resources
BOOKS
Darmstadt, Gary L., and Sidbury, Robert. "Diseases of the Epidermis." In Nelson Textbook of Pediatrics , 17th ed. Edited by Richard E. Behrman, et al. Philadelphia: Saunders, 2003, pp. 2195-9.
Genital Warts: A Medical Dictionary, Bibliography, and Annotated Research Guide to Internet References. San Diego, CA: ICON Health Publications, 2003.
Plantar Warts: A Medical Dictionary, Bibliography, and Annotated Research Guide to Internet References. San Diego, CA: ICON Health Publications, 2003.
Royston, Angela. Warts. London: Heinemann, 2001.
Swerlick, Robert A., and Lawley, Thomas J. "Eczema, Psoriasis, Cutaneous Infections, Acne, and Other Common Skin Disorders." In Harrison's Principles of Internal Medicine , 15th ed. Edited by Eugene Braunwald, et al. New York: McGraw-Hill, 2001, pp. 309–14.
Warts: A Medical Dictionary, Bibliography, and Annotated Research Guide to Internet References. San Diego, CA: ICON Health Publications, 2003.
PERIODICALS
Bellew, S. G., et al. "Childhood warts: an update." Cutis 73 (2004): 379–84.
Clemons, R. J., et al. "Comparing therapy costs for physician treatment of warts." Journal of Drugs in Dermatology 2 (2004): 649–54.
Laube, S. "Skin infections and ageing." Ageing Research Reviews 3 (2004): 69–89.
Silverberg, N. B. "Human papillomavirus infections in children." Current Opinions in Pediatrics 16 (2004): 402–9.
Tucker, S. B., et al. "Plantar wart treatment with combination imiquimod and salicylic acid pads." Journal of Drugs in Dermatology 2 (2003): 124–6.
ORGANIZATIONS
American Academy of Dermatology. 930 N. Meacham Road, PO Box 4014, Schaumburg, IL 60168–4014. Web site: http://www.aad.org/.
American Academy of Family Physicians. 11400 Tomahawk Creek Parkway, Leawood, KS 66211–2672. Web site: http://www.aafp.org/.
American Academy of Pediatrics. 141 Northwest Point Boulevard, Elk Grove Village, IL 60007–1098. Web site: http://www.aap.org/default.htm.
American Association of Naturopathic Physicians. 8201 Greensboro Drive, Suite 300, McLean, VA 22102. Web site: http://naturopathic.org/ .
American College of Physicians. 190 N Independence Mall West, Philadelphia, PA 19106–1572. Web site: http://www.acponline.org/.
American Podiatric Medical Association. 9312 Old Georgetown Road Bethesda, MD 20814–1698. Web site: http://www.apma.org/.
WEB SITES
"Human Papillomavirus and Genital Warts." National Institute of Allergy and Infectious Disease , July 2004. Available online at http://www.niaid.nih.gov/factsheets/stdhpv.htm (accessed December 4, 2005).
"Warts." American Academy of Family Physicians. Available online at http://familydoctor.org/209.xml (accessed December 4, 2005).
"Warts." National Library of Medicine. Available online at http://www.nlm.nih.gov/medlineplus/warts.html (accessed December 4, 2005).
"Warts." University of Illinois. Available online at http://www.mckinley.uiuc.edu/health-info/dis-cond/warts/warts.html (accessed December 4, 2005).
"What are plantar warts?" American Podiatric Medical Association. Available online at http://www.apma.org/topics/Warts.htm (accessed December 4, 2005).
L. Fleming Fallon, Jr., MD, DrPH
Comment about this article, ask questions, or add new information about this topic: