Tetralogy of Fallot
Definition
Tetralogy of Fallot is a common syndrome of congenital heart defects.
Description
The heart is two pumps in one. The ventricle on the left side pumps blood full of oxygen through the body; the ventricle on the right side pumps the same blood through the pulmonary artery to the lungs to take up oxygen. The left ventricle operates at pressures about four times as high as the right ventricle. Blood is supposed to flow through one side, then the other.
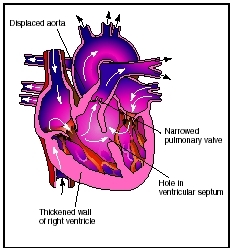
Tetralogy of Fallot is a condition that is characterized by several congenital heart defects occurring at once. They include: ventricular septal defect (abnormal passageway between the right and left ventricles), displaced aorta, narrowed pulmonary valve, thickened right ventricle wall.
Each defect acts in combination with the others to create a malfunction of the heart. The problem starts very early in the uterus with a narrowed pulmonary valve and a hole between the ventricles. This is not particularly a problem for a fetus because hardly any blood flows through the lungs until birth. It is only after birth that the defects pose a problem. The blood that is supposed to start flowing through the lungs cannot easily get there because of the narrowed valve; however, the hole between the ventricles remains open. Because of the opening between ventricles, much of the blood that comes back to the heart needing oxygen is sent out without being properly oxygenated. In addition, the right heart has to pump at the same pressure as the left side. Several changes follow. First, the baby turns blue (cyanotic) because of the deoxygenated blood that bypasses the lungs. Deoxygenated blood is darker and appears blue through the skin. Second, the right side of the heart (ventricle) hypertrophies (gets more muscular) from the extra exercise demanded of it. Next, the low oxygen causes the blood to get thicker and clot more easily. Clots in the veins can now pass through the hole in the heart and directly enter the aorta, where they can do much more damage than in the lungs such as causing infarcts in the brain. In addition, these anomalies make the lining of the heart more susceptible to infection (endocarditis), which can damage valves and lead to blood poisoning (septicemia).
Demographics
Researchers estimate that tetralogy of Fallot occurs in approximately one in every 2000 births. In the United States, almost 10 percent of congenital heart disease is tetralogy of Fallot. Boys are slightly more likely to have this malformation than girls.
Causes and symptoms
Tetralogy of Fallot is a congenital defect with unknown causes. Babies with tetralogy of Fallot are blue at birth or cyanotic. Sometimes the blue color appears only when they cry. They also have detectable heart murmurs . Infants with mild forms can have surgery postponed until they are older. Infants with more severe symptoms often have attacks of worsened cyanosis. During attacks, they turn very blue, have shortness of breath, and can faint. These symptoms usually occur during heightened activity, such as crying.
Diagnosis
A complete evaluation of the circulation is required, testing the blood for its oxygen content. Three diagnostic tests are performed: an echocardiogram, a chest x ray, and an electrocardiogram.
Treatment
Correction of the defects is done through open heart surgery. Surgery must be carefully timed with attention to the progression of the disease process, the size of the infant,
During surgery, the pulmonary valve is widened, the ventricular septal defect is closed, and any interim correction is removed.
Prognosis
Surgical correction has a high rate of success, returning the child to near-normal health.
Prevention
There is no known prevention for tetralogy of Fallot.
Parental concerns
Tetralogy of Fallot is a complex congenital malformation; however, open heart surgery is highly effective in correcting it. Most children have an excellent outcome and a normal healthy life. For most children, activity level, appetite, and growth eventually return to normal. Open heart surgery to repair tetralogy of Fallot is usually performed in children between the ages of six months and two years. Children with severe tetralogy of Fallot will begin the process of surgical correction in infancy. For children in whom the condition is milder, corrective surgery may be postponed until the child is older and has grown. While waiting for corrective surgery, children may experience episodes called paroxysmal hypercyanotic attacks, in which the child may cry intensely or become restless, turn blue (especially around the lips, fingernails, and toenails), and sometimes faint. These attacks can be quite serious and may require emergency medical care. For infants, holding the baby on the parent's shoulder with the infant's knees tucked underneath him may help reduce the symptoms. Older children may crouch in a squatting position.
KEY TERMS
Aorta —The main artery located above the heart that pumps oxygenated blood out into the body. The aorta is the largest artery in the body.
Cyanotic —Marked by a bluish tinge to the skin that occurs when the blood oxygen level drops too low. It is one of the types of congenital heart disease.
Deoxygenated blood —Blood that does not contain oxygen.
Endocarditis —Inflammation of the inner membrane lining heart and/or of the heart valves caused by infection.
Infarct —An area of dead tissue caused by inadequate blood supply.
Paroxysmal hypercyanoic attacks —Sudden episodes of cyanosis resulting from the circulation of deoxygenated blood to the body.
Septicemia —A systemic infection due to the presence of bacteria and their toxins in the bloodstream. Septicemia is sometimes called blood poisoning.
Systemic circulation —Refers to the general blood circulation of the body, not including the lungs.
Ventricles —The lower pumping chambers of the heart. The ventricles push blood to the lungs and the rest of the body.
After the child's heart surgery, parents should follow all instructions given by the healthcare team. Most children will continue to be seen by a team of doctors including the pediatrician, cardiologist, and pediatric cardiac surgeon.
When to call the doctor
Following open heart surgery, parents should call the doctor if any of the following occurs:
- fever of 101.5°F (38.6°C) or higher
- swelling or puffiness around the child's eyes, arms, or legs
- redness or swelling, cloudy yellow drainage, or an opening at the incision site
- rapid breathing
- increased fatigue or tiredness
- dry cough that was not present before surgery
- decreased appetite or refusal to eat
- increased pain
Resources
BOOKS
Behrman, Richard E., Robert M. Kliegman, and Hal B. Jenson. Nelson Textbook of Pediatrics , 16th ed. Philadelphia: Saunders, 2000.
Rudolph, Colin D., and Abraham M. Rudolph, eds. Rudolph's Pediatrics , 21st ed. New York: McGraw-Hill, 2003.
WEB SITES
C. S. Mott Children's Hospital. "Home Care after Heart Surgery." Available online at http://www.med.umich.edu/1libr/chheart/care10.htm (accessed August 11, 2004).
J. Ricker Polsdorfer, MD Deborah L. Nurmi, MS
Comment about this article, ask questions, or add new information about this topic: