Strep throat
Definition
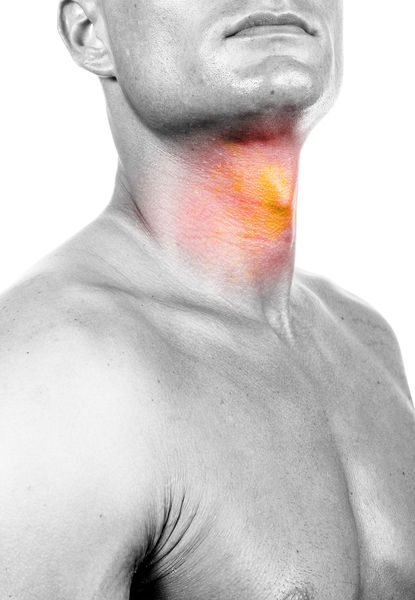
Streptococcal sore throat , or strep throat, as it is more commonly called, is a bacterial infection of the mucous membranes lining the throat or pharynx.
Description
Strep throat is caused by a type of bacteria called group A streptococci. The tonsils may also become infected ( tonsillitis ). Left untreated, strep throat may develop into rheumatic fever or other serious conditions.
Demographics
Strep throat accounts for between 5 and 10 percent of all sore throats. Although anyone can get strep throat, it is most common in school-age children. People who smoke, who are fatigued, run down, or who live in damp, crowded conditions are also more likely to become infected. Children under age two and adults who are not around children are less likely to get the disease.
Strep throat occurs most frequently between November to April. The disease passes directly from person to person by coughing, sneezing, and close contact. On rare occasions, the disease is passed through food, when a food handler infected with strep throat accidentally contaminates food by coughing or sneezing. Statistically, if someone in the household is infected, one out of every four other household members may get strep throat within two to seven days.
Causes and symptoms
A person with strep throat suddenly develops a painful sore throat one to five days after being exposed to the streptococcus bacteria. The pain is indistinguishable from sore throats caused by other diseases.
The infected person usually feels tired and has a fever , sometimes accompanied by chills, headache , muscle aches, swollen lymph glands, and nausea . Young children may complain of abdominal pain. The tonsils look swollen and are bright red, with white or yellow patches of pus on them. Sometimes the roof of the mouth is red or has small red spots. Often a person with strep throat has bad breath.
Despite these common symptoms, strep throat can be deceptive. It is possible to have the disease and not show any of these symptoms. Many young children complain only of a headache and stomachache, without the characteristic sore throat.
Occasionally, within a few days of developing the sore throat, an individual may develop a fine, rough, sunburn-like rash over the face and upper body and have a fever of 101–104°F (38.3–40°C). The tongue becomes bright red, with a flecked, strawberry-like appearance. When a rash develops, this form of strep throat is called scarlet fever . The rash is a reaction to toxins released by the streptococcus bacteria. Scarlet fever is no more dangerous than strep throat and is treated the same way. The rash disappears in about five days. One to three weeks later, patches of skin may peel off, as might occur with a sunburn , especially on the fingers and toes.
Untreated strep throat can cause rheumatic fever. This is a serious illness, although it occurs rarely. One outbreak appeared in the United States in the mid-1980s. Rheumatic fever occurs most often in children between the ages of five and 15 and may have a genetic component, since it seems to run in families. Although the strep throat that causes rheumatic fever is contagious, rheumatic fever itself is not.
Rheumatic fever begins one to six weeks after an untreated streptococcal infection. The joints, especially the wrists, elbows, knees, and ankles become red, sore, and swollen. The infected person develops a high fever and possibly a rapid heartbeat when lying down, paleness, shortness of breath, and fluid retention. A red rash over the trunk may come and go for weeks or months. An acute attack of rheumatic fever lasts about three months.
Rheumatic fever can cause permanent damage to the heart and heart valves. It can be prevented by promptly treating streptococcal infections with antibiotics . It does not occur if all the streptococcus bacteria are killed within the first ten to 12 days after infection.
In the 1990s, outbreaks of a virulent strain of group A streptococcus were reported to cause a toxic-shock-like illness and a severe invasive infection called necrotizing fasciitis, which destroys skin and muscle tissue. Although these diseases are caused by group A streptococci, they rarely begin with strep throat. Usually the streptococcus bacteria enters the body through a skin wound. These complications are rare. However, since the death rate in necrotizing fasciitis is 30 to 50 percent, it is wise to seek prompt treatment for any streptococcal infection.
Diagnosis
Diagnosis of a strep throat by a doctor begins with a physical examination of the throat and chest. The doctor will also look for signs of other illness, such as a sinus infection or bronchitis , and seek information about whether the patient has been around other people with strep throat. If it appears that the patient may have strep throat, the doctor will do laboratory tests.
There are two types of tests to determine if a person has strep throat. A rapid strep test can only determine the presence of streptococcal bacteria but will not tell if the sore throat is caused by another kind of bacteria. To perform a rapid strep test or a throat culture , a nurse will use a sterile swab to reach down into the throat and obtain a sample of material from the sore area. The procedure takes only a few seconds but may cause gagging. The results are available in about 20 minutes. The advantage of this test is the speed with which a diagnosis can be made.
The rapid strep test has a false negative rate of about 20 percent. In other words, in about 20 percent of cases where no strep is detected by the rapid strep test, the patient actually does have strep throat. Because of this margin of error, when a rapid strep test is negative, the doctor often does a throat culture.
For a throat culture a sample of swabbed material is cultured, or grown, in the laboratory on a medium that allows technicians to determine what kind of bacteria are present. Results take 24 to 48 hours. The test is very accurate and will show the presence of other kinds of bacteria besides streptococci. It is important not to take any leftover antibiotics before visiting the doctor and having a throat culture. Even small amounts of antibiotics can suppress the bacteria and mask its presence in the throat culture.
In the event that rheumatic fever is suspected, the doctor does a blood test. Results of this test, called an antistreptolysin-O test, tell the doctor whether the person has recently been infected with strep bacteria. This information helps the doctor distinguish between rheumatic fever and rheumatoid arthritis.
Treatment
Strep throat is treated with antibiotics. Penicillin is the preferred medication. Oral penicillin must be taken for 10 days. Patients need to take the entire amount of antibiotic prescribed and not discontinue taking the medication when they feel better. Stopping the antibiotic early can lead to a return of the strep infection. Occasionally, a single injection of long-acting penicillin (Bicillin) is given instead of ten days of oral treatment.
About 10 percent of the time, penicillin is not effective against the strep bacteria. When this happens a doctor may prescribe other antibiotics such as amoxicillin (Amoxil, Pentamox, Sumox, Trimox), clindamycin (Cleocin), or a cephalosporin (Keflex, Durocef, Ceclor). Erythromycin (Eryzole, Pediazole, Ilosone), another inexpensive antibiotic, is given to people who are allergic to penicillin. Scarlet fever is treated with the same antibiotics as strep throat.
Without treatment, the symptoms of strep throat begin subsiding in four or five days. However, because of the possibility of getting rheumatic fever, it is important to treat strep throat promptly with antibiotics. If rheumatic fever does occur, it is also treated with antibiotics. Anti-inflammatory drugs, such as steroids, are used to treat joint swelling. Diuretics are used to reduce water retention. Once the rheumatic fever becomes inactive, children may continue on low doses of antibiotics to prevent a reoccurrence. Necrotizing fasciitis is treated with intravenous antibiotics.
Prognosis
Patients with strep throat begin feeling better about 24 hours after starting antibiotics. Symptoms rarely last longer than five days.
People remain contagious until after they have been taking antibiotics for 24 hours. Children should not return to school or childcare until they are no longer contagious. Food handlers should not work for the first 24 hours after antibiotic treatment, because strep infections are occasionally passed through contaminated food. People who are not treated with antibiotics can continue to spread strep bacteria for several months.
About 10 percent of strep throat cases do not respond to penicillin. People who have even a mild sore throat after a 10-day treatment with antibiotic should return to their doctor. An explanation for this problem may be that the person is just a carrier of strep and that something else is causing the sore throat.
Taking antibiotics within the first week of a strep infection will prevent rheumatic fever and other complications. If rheumatic fever does occur, the outcomes vary considerably. Some cases may be cured. In others there may be permanent damage to the heart and heart valves. In rare cases, rheumatic fever can be fatal.
Necrotizing fasciitis has a death rate of 30 to 50 percent. Patients who survive often suffer a great deal of tissue and muscle loss. Fortunately, this complication of a streptococcus infection is very rare.
Prevention
There is no way to prevent getting a strep throat. However, the risk of getting one or passing one on to another person can be minimized by the following precautions:
- washing hands well and frequently, especially after nose blowing or sneezing and before food handling
- disposing of used tissues properly
- avoiding close contact with someone who has a strep throat
- not sharing food and eating utensils with anyone
- not smoking
Parental concerns
Children who have strep throat should be kept out of daycare, school, activities, and other public places until they have been taking their antibiotic for a full 24 hours. This will help decrease the likelihood of passing on the infection to others.
Parents who are caring for a child with strep will want to take the following steps:
- Give the child acetaminophen or ibuprofen for pain. Aspirin should not be given to children because of its association with Reye's syndrome , a serious disease.
- Encourage the child to gargle with warm double strength tea or warm salt water, made by adding one teaspoon of salt to eight ounces of water, to relieve sore throat pain.
- Make sure that the child drinks plenty of fluids but avoids acidic juices like orange juice because they irritate the throat.
- Offer the child soft, nutritious foods like noodle soup and avoid spicy foods.
- Help the child avoid exposure to people who are smoking.
- Encourage the child to rest until the fever is gone, then allow him or her to gradually resume activities.
- Use a room humidifier, as it may make sore throat sufferers more comfortable.
- Be aware that antiseptic lozenges and sprays may aggravate the sore throat rather than improve it.
KEY TERMS
Lactobacillus acidophilus —Commonly known as acidophilus, a bacteria found in yogurt that changes the balance of the bacteria in the intestine in a beneficial way.
Resources
BOOKS
Gerber, Michael A. "Group A Streptococcus." In Nelson Textbook of Pediatrics. Edited by Richard E. Behrman et al. Philadelphia: Saunders, 2004.
PERIODICALS
Ebell, M. H. "Strep Throat." American Family Physician 68 (September 1, 2000): 937–8.
Tish Davidson, A.M. Rosalyn Carson-DeWitt, MD
Comment about this article, ask questions, or add new information about this topic: