Ringworm
Definition
Ringworm is a common fungal infection of the skin. The name is a misnomer because the disease is not caused by a worm.
Description
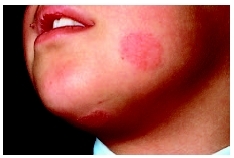
Ringworm is characterized by patches of rough, reddened skin. Raised eruptions usually form the circular pattern that gives the condition its name. As lesions grow, the centers start to heal. The inflamed borders expand and spread the infection. Ringworm may also be referred to as dermatophyte infection. It is more common in males than females, and is most common among children ages three to nine years.
Types of ringworm
Ringworm is a term that is commonly used to encompass several types of fungal infection. Sometimes, however, only body ringworm is classified as true ringworm.
Body ringworm (tinea corporis) can affect any part of the body except the scalp, feet, and facial area where a man's beard grows. The well-defined, flaky sores can be dry and scaly or moist and crusty.
Scalp ringworm (tinea capitis) is most common in children. It causes scaly, swollen blisters or a rash that looks like black dots. Sometimes inflamed and filled with pus, scalp ringworm lesions can cause crusting, flaking, and round bald patches. Most common in black children, scalp ringworm can cause scarring and permanent hair loss.
Ringworm of the groin (tinea cruris or jock itch) produces raised red sores with well-marked edges. It can spread to the buttocks, inner thighs, and external genitals.
Ringworm of the nails (tinea unguium) generally starts at the tip of one or more toenails, which gradually thicken and discolor. The nail may deteriorate or pull away from the nail bed. Fingernail infection is far less common.
Demographics
Ringworm can affect people at any age. It is more common among children, athletes, and people with poor hygiene habits.
Causes and symptoms
Ringworm can be transmitted by infected people or pets or by towels, hairbrushes, or other objects contaminated by them. Symptoms include inflammation, scaling, and sometimes, itching .
Diabetes mellitus increases susceptibility to ringworm. Dampness, humidity, and dirty, crowded living areas also increase susceptibility. Braiding hair tightly and using hair gel also raise the risk.
When to call the doctor
A health professional should be consulted when signs of ringworm appear or if exposure to someone with ringworm is suspected.
Diagnosis
Diagnosis is based on microscopic examination of scrapings taken from lesions. A dermatologist may also study the scalp of a person with suspected tinea capitis under ultraviolet light.
Treatment
Some infections disappear without treatment. Others respond to such topical antifungal medications as naftifine (Caldesene Medicated Powder) or tinactin (Desenex) or to griseofulvin (Fulvicin), which is taken by mouth. Medications should be continued for two weeks after lesions disappear.
A person with body ringworm should wear loose clothing and check daily for raw, open sores. Wet dressings applied to moist sores two or three times a day can lessen inflammation and loosen scales. The doctor may suggest placing special pads between folds of infected skin, and anything the person has touched or worn should be sterilized in boiling water.
Infected nails should be cut short and straight and carefully cleared of dead cells with an emery board.
People with jock itch should:
- wear cotton underwear and change it more than once a day
- keep the infected area dry
- apply antifungal ointment over a thin film of antifungal powder
Shampoo containing selenium sulfide can help prevent spread of scalp ringworm, but prescription shampoo or oral medication is usually needed to cure the infection.
Alternative treatment
The fungal infection ringworm can be treated with homeopathic remedies. Among the homeopathic remedies recommended are:
- sepia for brown, scaly patches
- tellurium for prominent, well-defined, reddish sores
- graphites for thick scales or heavy discharge
- sulfur for excessive itching
Topical applications of antifungal herbs and essential oils also can help resolve ringworm. Tea tree oil ( Melaleuca spp.), thuja ( Thuja occidentalis ), and lavender ( Lavandula officinalis ) are the most common. Two drops of essential oil in 0.25 oz (7 ml) of carrier oil is the dose recommended for topical application. Essential oils should not be applied to the skin undiluted. Botanical medicine can be taken internally to enhance the body's immune response. A person must be susceptible to exhibit this overgrowth of fungus on the skin. Echinacea ( Echinacea spp.) and astragalus ( Astragalus membranaceus ) are the two most common immune-enhancing herbs. A well-balanced diet, including protein, complex carbohydrates, fresh fruits and vegetables, and good quality fats, is also important in maintaining optimal immune function.
Prognosis
Ringworm can usually be cured, but recurrence is common. Chronic infection develops in one person in five.
It can take six to 12 months for new hair to cover bald patches, and three to 12 months to cure infected fingernails. Toenail infections do not always respond to treatment.
Prevention
Likelihood of infection can be lessened by avoiding contact with infected people or pets or contaminated objects and staying away from hot, damp places.
Parental concerns
Parents should monitor the children with whom their own children interact or play . Children should not be allowed to play with other children who have open skin sores or scratch excessively.
KEY TERMS
Dermatophyte —A type of fungus that causes diseases of the skin, including tinea or ringworm.
Diabetes mellitus —The clinical name for common diabetes. It is a chronic disease characterized by the inability of the body to produce or respond properly to insulin, a hormone required by the body to convert glucose to energy.
Resources
BOOKS
Bennett, John C. "Diagnosis and Treatment of Fungal Infections." In Harrison's Principles of Internal Medicine. 15th ed. Ed. by Eugene Braunwald et al., New York, McGraw Hill, 2001, 1168–70.
Darmstadt, Gary L and Sidbury, Robert. "Diseases of the Epidermis." In Nelson Textbook of Pediatrics. 17th ed. Ed. by Richard E. Behrman, et al., Philadelphia: Saunders, 2003, 2195–9.
PERIODICALS
Gupta, A.K., et al. "Optimal management of fungal infections of the skin, hair, and nails." American Journal of Clinical Dermatology 5, no. 4 (2004): 225-37.
McLeod, R.P. "Lumps, bumps, and things that go itch in your office!" Journal of School Nursing 20, no. 2 (2004): 115-6.
Sladden, M.J. and G.A. Johnston. "Common skin infections in children." British Medical Journal 329, no. 7457 (2004): 95-9.
ORGANIZATIONS
American Academy of Dermatology, 930 N. Meacham Road, PO Box 4014, Schaumburg, IL 60168-4014. (847) 330-0230. Fax: (847) 330-0050. Web site: http://www.aad.org.
WEB SITES
"Ringworm on Scalp." eMedicine. Available online at: http://www.emedicinehealth.com/articles/15983-1.asp.
"Ringworm." Directors of Health Promotion and Education. Available online at: http://www.astdhpphe.org/infect/ringworm.html.
"Tinea." Kid's Health. Available online at: http://kidshealth.org/parent/infections/fungal/ringworm.html.
L. Fleming Fallon, Jr., MD, DrPH
Comment about this article, ask questions, or add new information about this topic: