Psoriasis
Definition
Named for the Greek word psōra meaning itch, psoriasis is a chronic, non-contagious disease characterized by inflamed lesions covered with silvery-white scabs of dead skin.
Description
Normal skin cells mature and replace dead skin every 28 to 30 days. In psoriasis, the immune system triggers the immune system to make T cells, a type of white blood cell, that cause skin cells to mature in two to three days. Because the body cannot shed old skin as rapidly as the new cells appear, raised patches of dead skin form on the body.
Psoriasis is considered mild if it affects less than 5 percent of the surface of the body; moderate, if 5 to 30 percent of the skin is involved, and severe, if the disease affects more than 30 percent of the body surface.
There is no cure for psoriasis. The disease is managed through treatment. Psoriasis can seriously impact children's lives when the hands and feet are affected so the children cannot take notes or walk or play , or when the disease becomes so widespread that the immune system becomes compromised. Children also experience low self-esteem and depression because of the disfiguring aspects of the disease.
Types of psoriasis
Dermatologists distinguish different forms of psoriasis according to what part of the body is affected, how severe symptoms are, how long they last, and the pattern formed by the scales. Though children usually have only one form of the disease, some do experience two more types of psoriasis throughout their lifetimes.
PLAQUE PSORIASIS Plaque psoriasis (psoriasis vulgaris), the most common form of the disease, is characterized by small, red bumps that enlarge, become inflamed, and form scales. The top scales flake off easily and often, but those beneath the surface of the skin clump together. Removing these scales exposes tender skin, which bleeds and causes the plaques (inflamed patches of skin) to grow.
Plaque psoriasis can develop on any part of the body, but most often occurs on the elbows, knees, scalp, and trunk. Patches of psoriasis are found in the scalp for nearly half of all psoriasis sufferers.
GUTTATE PSORIASIS Named for the Latin word gutta , which means "a drop," guttate psoriasis is characterized by small, red, drop-like dots that enlarge rapidly and may be somewhat scaly. Often found on the arms, legs, trunk, scalp, and sometimes in the diaper area, guttate psoriasis can clear up without treatment or disappear and resurface in the form of plaque psoriasis.
Guttate psoriasis is the most common form of psoriasis in children. It usually first appears in children around four or five years old after a streptococcal infection.
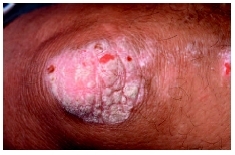
PUSTULAR PSORIASIS Pustular psoriasis usually occurs in adults but can occur in children and adolescents. It is characterized by blister-like lesions filled with non-infectious pus and surrounded by reddened skin. Pustular psoriasis, which can be limited to one part of the body or can be widespread, may be the first symptom of psoriasis or develop in a patient with chronic plaque psoriasis.
Generalized pustular psoriasis is also known as Von Zumbusch pustular psoriasis. Widespread, acutely painful patches of inflamed skin develop suddenly. Pustules appear within a few hours, then dry, and peel within two days. It can make life-threatening demands on the heart and kidneys.
Palomar-plantar pustulosis (PPP) generally appears between the ages of 20 and 60.
INVERSE PSORIASIS Inverse psoriasis occurs in the armpits and groin, under the breasts, and in other areas where skin flexes or folds. This disease is characterized by smooth, inflamed lesions and can be debilitating.
ERYTHRODERMIC PSORIASIS Characterized by severe scaling, itching , and pain that affects most of the body, erythrodermic psoriasis disrupts the body's chemical balance and can cause severe illness or even death when the body's immune system becomes compromised. Erythrodermic psoriasis interferes with the body's ability to control temperature and prevent infections. This particularly inflammatory form of psoriasis can be the first sign of the disease but often develops in patients with a history of plaque psoriasis.
PSORIATIC ARTHRITIS About 10 percent of patients with psoriasis develop a complication called psoriatic arthritis. This type of arthritis can be slow to develop and mild, or it can develop rapidly. Symptoms of psoriatic arthritis include:
- joint discomfort, swelling, stiffness, or throbbing
- swelling in the toes and ankles
- pain in the digits, lower back, wrists, knees, and ankles
- eye inflammation or pink eye (conjunctivitis)
Children who have psoriatic arthritis also have nail deformations, usually pitting of the fingernails or toenails. Size, shape, and depth of the marks vary, and affected nails may thicken, yellow, or crumble. The skin around an affected nail is sometimes inflamed, and the nail may peel away from the nail bed.
Demographics
Psoriasis affects 4.5 million Americans and is slightly more common in women than in men. Although the disease can develop at any time, a third of all cases occur in childhood with 10 to 15 percent of them being diagnosed in children under ten. It appears between the ages of 15 and 35. It is rare in infants but does occur. Nearly 20,000 U.S. children are diagnosed with psoriasis every year. Psoriasis affects people of all ethnicities, but fair-skinned individuals have a slightly higher incidence.
About 1.5 million Americans have moderate to severe psoriasis. Of them, 75 percent report that their disease has a serious impact on their daily lives. One-third report sleeping problems, disruptions with their normal routine, and negative self-image because of the disease.
In adults, psoriasis can be serious enough that four hundred people are granted disability by the Social Security Administration each year, and having psoriasis disqualifies individuals from serving in the military. Annually, three hundred and fifty people die annually from psoriasis or complications of treatment.
Nearly one million people in the United States have psoriatic arthritis. Though psoriatic arthritis usually develops between the age of 30 and 50, it does occur in children. About 10 to 30 percent of psoriasis patients have psoriatic arthritis, but the condition can occur before the characteristic scaly lesions occur.
Having one parent with psoriasis increases a child's risk of developing the disease to 20 to 25 percent. If both parents have psoriasis, the risk is doubled.
Patients with psoriasis make 2.4 million visits to dermatologists each year, with costs exceeding $3 million annually.
Causes and symptoms
Causes
The cause of psoriasis is, as of 2004, unknown, but research suggests that it is genetic and is related to the immune-system. Having both parents with the disease increases a child's risk by 50 percent.
Psoriasis is usually cyclical, with episodes flaring up for weeks or months throughout the child's life and then receding. Certain factors, however, do seem to trigger bouts of the disease. Injury to the skin seems to precipitate many episodes of plaque psoriasis, usually within seven to ten days. This is called the Koebner reaction. Streptococcal infections are associated with guttate psoriasis and some plaque psoriasis cases. Both trauma and certain bacteria may also trigger psoriatic arthritis.
Environmental factors are also implicated in reoccurrence of psoriasis. Exposure to cold temperatures can trigger episodes of the disease. Though sunlight is usually beneficial to most patients, for a few children, too much sun can cause a flare up or worsen the condition.
Some drugs have been found to aggravate psoriasis. Antimalarial drugs, beta-blockers used to treat high blood pressure, and lithium, a drug used to treat depression and bi-polar disorder, can make episodes worse in some individuals. Non-steroid anti-inflammatory (NSAID) drugs, such as ibuprofen or naproxen used to
During puberty , adolescents report more frequent flare ups and more severe ones. The hormonal changes within their bodies seem to trigger the immune system.
Stress is also a factor in increased frequency of psoriatic episodes. Because stress pumps large amounts of adrenalin, a hormone, into the body, the immune system is overstimulated and reacts by triggering flare ups of the disease.
Symptoms
The most common symptoms of psoriasis are skin rashes or red patches covered with white scales that may itch or burn. In plaque psoriasis, the skin may crack and bleed and is susceptible to infection. When the scales are removed, the skin underneath is deep red and shiny and may bleed. Psoriasis on the scalp is distinguished from seborrheic dermatitis , or dandruff, because the scales of psoriasis are dry, not greasy. There may be a red drop-like rash (guttate psoriasis) or patches of scaly skin that crack and ooze pus (pustular psoriasis).
In young children, the scaly patches in plaque psoriasis do not appear as thick or as scaly as those of adults. Psoriasis appears often in the diaper area and affects the face more in children than adolescents or adults.
When to call the doctor
Many children routinely see their doctors to supervise their regime of treatment for psoriasis flare ups. Others only see their doctors at the first sign of a recurrence of the disease. There are circumstances, however, when the doctor should be notified. If a treatment does not seem to be working, episodes worsen with treatment, or the child experiences a serious side effect to medications give, the doctor should be consulted to discuss alternative treatment. If there are signs of infections, such as red streaks on the skin or pus, or if there is fever or increased pain, the doctor should be called immediately.
Diagnosis
A complete medical history and examination of the skin, nails, and scalp are the basis for a diagnosis of psoriasis. In some cases, a microscopic examination of skin cells is also performed.
Blood tests can distinguish psoriatic arthritis from other types of arthritis. Rheumatoid arthritis, in particular, is diagnosed by the presence of a particular antibody present in the blood. That antibody is not present in the blood of patients with psoriatic arthritis.
Treatment
Age, general health, lifestyle, and the severity and location of symptoms influence the type of treatment used to reduce inflammation and decrease the rate at which new skin cells are produced. Because the course of this disease varies with each individual, doctors must experiment with or combine different treatments to find the most effective therapy for a particular patient.
Treating children with this disease with drugs is problematic. Though treatment regimes have been developed that are effective on adults, research has not been conducted sufficiently on children, except in the area of psoriatic arthritis. Treatment in children is usually not aggressive because of their small, developing bodies. Long-term use can produce toxicity so potent drugs, such as methotrexate (MTX) and cyclosporine, are not used with children. Although MTX is sometimes used in extreme cases for brief amounts of time. Topical steriods are also not used on children because their bodies can absorb the steriods in the medication.
Mild psoriasis
Typically, steroid creams and ointments are commonly used to treat mild or moderate psoriasis in adults. These topical ointments are not generally used with children for mild psoriasis. However, new creams that are used in treating eczema appear to be effective in treating psoriasis as well and do not appear to have long-term problems. In addition, tazarotene (Tazorac), a drug approved by the United States Food and Drug Administration (FDA) in 1997, is proving to be effective for mild-to-moderate plaque psoriasis. This water-based gel has chemical properties similar to vitamin A.
A more subdued approach is undertaken with children who have less severe psoriasis. Brief daily doses of natural sunlight can significantly relieve most symptoms. Sunburn , however, has the opposite effect.
Moisturizers and bath oils are used to loosen scales, soften skin, and eliminate the itch. Adding a cup of oatmeal to a tub of bath water is also helpful. Salicylic acid (an ingredient in aspirin) can be used to remove dead skin or increase the effectiveness of other therapies.
Moderate psoriasis
Administered under medical supervision, ultraviolet light B (UVB) is used to control psoriasis that covers many areas of the body or that has not responded to topical preparations. Doctors combine UVB treatments with topical medications to treat some patients and sometimes prescribe home phototherapy, in which the parent administers the UVB treatments.
Tanning beds use ultraviolet A and produce a more intense experience. Adolescents should avoid tanning salons and should sunbathe but without tanning. Any sun exposure or UVB treatment should be coordinated with a dermatologist.
Severe psoriasis
Methotrexate (MTX), given as a pill or as an injection, is sometimes used in extreme cases to alleviate symptoms of severe psoriasis or psoriatic arthritis. Patients who take MTX must be carefully monitored to prevent liver damage.
Enbrel is another drug dermatologists prescribe for children. It appears to be very safe when used for long periods of time.
A new self-injected medication called efalizumab (Raptiva) has the potential to be effective for severe cases of psoriasis. Since it is suppresses the immune system, its use with children or over the long-term is cautioned because it can increase the risk of infection.
Psoriatic arthritis can also be treated with NSAIDs, such as acetaminophen (Tylenol) or aspirin. Hot compresses and warm water soaks may also provide some relief for painful joints.
Photochemotherapy (PUVA) is a medically supervised procedure that combines medication with exposure to ultraviolet light (UVA) to treat localized or widespread psoriasis. An individual with widespread psoriasis that has not responded to treatment may enroll in one of the day treatment programs conducted at special facilities throughout the United States. Psoriasis patients who participate in these intensive sessions are exposed to UVA and given other treatments for six to eight hours a day for two to four weeks.
Alternative treatment
Non-traditional psoriasis treatments include:
- soaking in warm water and German chamomile ( Matricaria recutita ) or bathing in warm salt water
- drinking as many as three cups a day of hot tea made with one or a combination of the following herbs: burdock ( Arctium lappa ) root, dandelion ( Taraxacum mongolicum ) root, Oregon grape ( Mahonia aquifolium ), sarsaparilla ( Smilax officinalis ), and balsam pear ( Momardica charantia )
- taking two 500-mg capsules of evening primrose ( Oenothera biennis ) oil a day (Pregnant women should not use evening primrose oil, and patients with liver disease or high cholesterol should use it only under a doctors supervision.)
- eating a diet that includes plenty of fish, turkey, celery (for cleansing the kidneys), parsley, lettuce, lemons (for cleansing the liver), limes, fiber, and fruit and vegetable juices
- eating a diet that eliminates animal products high in saturated fats, since they promote inflammation
- drinking plenty of water (at least eight glasses) each day
- taking nutritional supplements including folic acid , lecithin, vitamin A, vitamin E, selenium, and zinc
- regularly imagining clear, healthy skin
Other helpful alternative approaches include identifying and eliminating food allergens from the diet, enhancing the function of the liver, augmenting the hydrochloric acid in the stomach, and completing a detoxification program. Constitutional homeopathic treatment, if properly prescribed, can also help resolve psoriasis.
Prognosis
Most cases of psoriasis can be controlled, and most people who have psoriasis can live normal lives. However, some people who have psoriasis are so self-conscious and embarrassed about their appearance that they become depressed and withdrawn. Others may become disabled because of psoriatic arthritis or because their psoriasis affects their hands and feet so that they cannot walk or handle objects.
Prevention
Psoriasis cannot be prevented. However, recurrences can be avoided or minimized by maintaining a healthy lifestyle by getting plenty of sleep , eating a balanced diet, participating in regular exercise , and minimizing stress. Avoiding overexposure to cold temperatures, sunburn, and skin irritants, such as drying soaps and lotions, can also minimize flare-ups. Not smoking or drinking alcohol can also prevent or minimize some episodes.
Parental concerns
Children living with psoriasis often find the disease overwhelming. It is an emotionally charged disease that can have a child feeling anger one minute and deep depression the next. Because the disfigurement of their skin, though often temporary, is sometimes quite pronounced, children will turn inward, avoiding contact with friends or relatives. School can be particularly traumatizing due to teasing by other children. Teenagers, who already feel awkward and ugly, may feel worse during flare-ups of the disease. Complicating this already emotional situation is the discouragement of treatments that do not work as expected and the uncertainty of finding something that will work.
Parents can help their children by providing education about the psoriasis. This is the first step in managing the disease and feeling some control in their lives. Sometimes this education includes discussing the disease with the childs teachers or the parents of their friends so that these adults will understand more about the emotional state of the child.
Parents can listen to their children when they are able to talk about their feelings about the disease. Emphasizing their childrens strengths, especially when these children appear sad or depressed, and encouraging them to stay active and see their friends can help a child cope with the disease.
Sometimes, participating in a childrens psoriasis support group may be helpful. In addition, sending the child to a special camp for school age children with childhood skin diseases can help them learn tools for coping with the disease as well as establish a support system.
Children can often feel shame as well as guilt, thinking that they have somehow brought on the disease. Coupled with anger and resentment, these powerful emotions can contribute to stress, which can trigger the recurrence of the disease. Stress reduction techniques, such as exercise, yoga , and meditation, are also helpful.
Parents should be available to their child and offer as much tangible and emotional support they can. However, they should not encourage the child to become too dependent on the parent or others. Parents can also help children find creative solutions to deal with teasing, camouflage their lesions, and educate their peers about the disease. One of the most important lessons parents can teach their child, who is living with psoriasis, is not to be embarrassed because of the disease. Psoriasis can be treated matter-of-factly as people do diabetes, another chronic disorder.
KEY TERMS
Adrenaline —Another name for epinephrine, the hormone released by the adrenal glands in response to stress. It is the principal blood-pressure raising hormone and a bronchial and intestinal smooth muscles relaxant.
Arthritis —A painful condition that involves inflammation of one or more joints.
Plaque —Inflamed patches of skin present in some forms of psoriasis.
T cell —A type of white blood cell that is produced in the bone marrow and matured in the thymus gland. It helps to regulate the immune system's response to infections or malignancy.
See also Depressive disorders ; Itching ; Self-esteem .
Resources
BOOKS
Cram, David L. Coping with Psoriasis: A Patients Guide to Treatment. Omaha, NB: Addicus Books, 2000.
Scott, Jerry G. Psoriasis: The Real Way Out: A Self-Education Guide to Complete Natural Healing. Kenora, Ont.: Psoriasis Connection International, 2003.
PERIODICALS
"Generic Name: Efalizumab Injection." Drug Topics 148 (January 26, 2004): HSE21.
Harrar, Sari. "New, Inject-it-yourself." Prevention 56 (2004): 48.
ORGANIZATIONS
American Academy of Dermatology. 930 N. Meacham Road, PO Box 4014, Schaumburg, IL 601684014. Web site: http://www.aad.org.
American Skin Association Inc. 150 E. 58th St., 3rd floor, New York, NY 101550002. Web site: http://www.americanskin.org.
National Psoriasis Foundation. 6600 SW 92nd Ave., Suite 300, Portland, OR 97223. Web site: http://www.psoriasis.org.
WEB SITES
"Juvenile Psoriatic Arthritis." Arthritis Foundation , 2004. Available online at http://www.arthritis.org/conditions/diseasecenter/juvenilepsoriaticarthritis.asp(accessed December 11, 2004).
Janie Franz Maureen Haggerty
Comment about this article, ask questions, or add new information about this topic: