Obsessive-compulsive disorder
Definition
Obsessive-compulsive disorder (OCD) is a type of anxiety disorder. Anxiety disorder is the experience of prolonged, excessive worry about circumstances in one's life. OCD is characterized by distressing repetitive thoughts, impulses, or images that are intense, frightening, absurd, or unusual. These thoughts are followed by ritualized actions that are usually bizarre and irrational. These ritual actions, known as compulsions, help reduce anxiety caused by the individual's obsessive thoughts. Often described as the "disease of doubt," the sufferer usually knows the obsessive thoughts and compulsions are irrational but, on another level, fears they may be true.
Description
Most people with obsessive-compulsive disorder have both obsessions and compulsions, but occasionally a person will have just one or the other. The degree to which this condition can interfere with daily living also varies. Some people are barely bothered, while others find the obsessions and compulsions to be profoundly traumatic and spend much time each day in compulsive actions. Because the symptoms are so distressing, sufferers often hide heir fears and rituals but cannot avoid acting on them. OCD sufferers are often unable to decide if their fears are realistic and need to be acted upon.
Obsessions are intrusive, irrational thoughts that keep popping up in a person's mind, such as the urgency to wash one's hands again. Typical obsessions include fears of dirt, germs, contamination, and violent or aggressive impulses. Other obsessions include feeling responsible or others' safety or an irrational fear of hitting a pedestrian with a car. Additional obsessions can involve excessive religious feelings or intrusive sexual thoughts. The patient may need to confess frequently to a religious counselor or may fear acting out the strong sexual thoughts in a hostile way. People with obsessive-compulsive disorder may have an intense preoccupation with order and symmetry or may be unable to throw anything out.
Compulsions usually involve repetitive rituals such as excessive washing (especially hand washing or bathing), cleaning, checking and touching, counting, arranging, and/or hoarding. As the person performs these acts, he may feel temporarily better, but there is no long-lasting sense of satisfaction or completion after the act is performed. Often, a person with obsessive-compulsive disorder believes that if the ritual is not performed, something dreadful will happen. While these compulsions may temporarily ease stress, short-term comfort is purchased at a heavy price—time spent repeating compulsive actions and a long-term interference with life.
The difference between OCD and other compulsive behavior is that while people who have problems with gambling, overeating, or with substance abuse may appear to be compulsive, these activities also provide pleasure to some degree. The compulsions of OCD, on the other hand, are never pleasurable.
OCD may be related to some other conditions, such as the continual urge to pull out body hair ( trichotillomania ); fear of having a serious disease (hypochondriasis); or preoccupation with imagined defects in personal appearance disorder (body dysmorphia). Some people with OCD also have Tourette syndrome , a condition featuring tics and unwanted vocalizations (such as swearing). OCD is often linked with depression and other anxiety disorders.
Demographics
Almost one out of every 40 people suffers from obsessive-compulsive disorder at some time in their lives. The condition is two to three times more common than either schizophrenia or manic depression and strikes men and women of every ethnic group, age, and social level.
If one person in a family has obsessive-compulsive disorder, there is a 25 percent chance that another immediate family member has the condition. It also appears that stress and psychological factors may worsen symptoms, which usually begin during adolescence or early adulthood.
Causes and symptoms
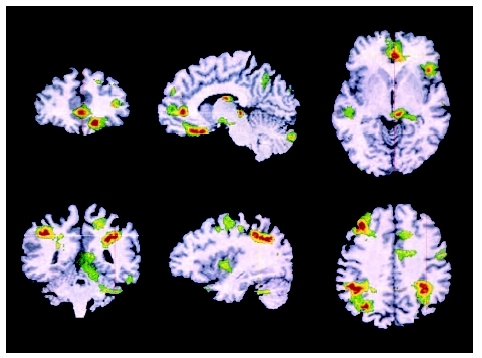
Research suggests that the tendency to develop obsessive-compulsive disorder is inherited. There are several theories behind the cause of OCD. OCD may be related to a chemical imbalance within the brain that causes a communication problem between the front part of the brain (frontal lobe) and deeper parts of the brain responsible for the repetitive behavior. The orbital cortex located on the underside of the brain's frontal lobe is overactive in OCD patients. This may be one reason for the feeling of alarm that pushes the patient into compulsive, repetitive actions. It is possible that people with OCD experience overactivity deep within the brain that causes the cells to get "stuck," much like a jammed transmission in a car damages the gears. This could lead to the development of rigid thinking and repetitive movements common to the disorder. The fact that drugs which boost the levels of serotonin, a brain messenger substance linked to emotion and many different anxiety disorders, in the brain can reduce OCD symptoms may indicate that to some degree OCD is related to levels of serotonin in the brain.
There may also be a link between childhood episodes of strep throat and the development of OCD. In some vulnerable children, strep antibodies attack a certain part of the brain. Antibodies are cells that the body produces to fight specific diseases. That attack results in
Diagnosis
People with obsessive-compulsive disorder feel ashamed of their problem and often try to hide their symptoms. They avoid seeking treatment. Because they can be very good at keeping their problem from friends and family, many sufferers do not get the help they need until the behaviors are deeply ingrained habits and hard to change. As a result, the condition is often misdiagnosed or underdiagnosed. All too often, it can take more than a decade between the onset of symptoms and proper diagnosis and treatment.
OCD appears to be related to a disruption in serotonin levels, there is no blood test for the condition. Instead, doctors diagnose OCD after evaluating a person's symptoms and history.
Treatment
Obsessive-compulsive disorder can be effectively treated by a combination of cognitive-behavioral therapy and medication that regulates the brain's serotonin levels. Drugs that are approved to treat obsessive-compulsive disorder include fluoxetine (Prozac), fluvoxamine (Luvox), paroxetine (Paxil), and sertraline (Zoloft), all selective serotonin reuptake inhibitors (SSRIs) that affect the level of serotonin in the brain. Older drugs include the antidepressant clomipramine (Anafranil), a widely studied drug in the treatment of OCD, but one that carries a greater risk of side effects. Drugs should be taken for at least 12 weeks before a person decides whether they are effective.
Cognitive-behavioral therapy (CBT) teaches patients how to confront their fears and obsessive thoughts by making the effort to endure or wait out the activities that usually cause anxiety without compulsively performing the calming rituals. Eventually their anxiety decreases. People who are able to alter their thought patterns in this way can lessen their preoccupation with the compulsive rituals. At the same time, the patient is encouraged to refocus attention elsewhere, such as on a hobby.
In a few very severe cases in which patients have not responded to medication or behavioral therapy, brain surgery may be tried as a way of relieving the unwanted symptoms. Surgery can help up to one third of patients with the most severe form of OCD. The most common operation involves removing a section of the brain called the cingulate cortex. The serious side effects of this surgery for some patients are seizures, personality changes, and less ability to plan.
Prognosis
Obsessive-compulsive disorder is a chronic disease that, if untreated, can last for decades, fluctuating from mild to severe and worsening with age. When treated by a combination of drugs and behavioral therapy, some patients go into complete remission. Unfortunately, not all patients have such a good response. About 20 percent of people cannot find relief with either drugs or behavioral therapy. Hospitalization may be required in some cases.
Despite the crippling nature of the symptoms, many successful doctors, lawyers, business people, performers, and entertainers function well in society despite their condition. Nevertheless, the emotional and financial cost of obsessive-compulsive disorder can be quite high.
Parental concerns
Some people have referred to obsessive-compulsive disorder as "the great pretender," because its symptoms can mimic a number of other disorders. Furthermore, children may become skilled at hiding the more embarrassing features of their condition. Because of these characteristics of the disorder, obsessive-compulsive disorder may go undiagnosed for some time.
KEY TERMS
Anxiety disorder —A mental disorder characterized by prolonged, excessive worry about circumstances in one's life. Anxiety disorders include agoraphobia and other phobias, obsessive-compulsive disorder, post-traumatic stress disorder, and panic disorder.
Cognitive-behavioral therapy —A type of psychotherapy in which people learn to recognize and change negative and self-defeating patterns of thinking and behavior.
Compulsion —A repetitive or ritualistic behavior that a person performs to reduce anxiety. Compulsions often develop as a way of controlling or "undoing" obsessive thoughts.
Obsession —A persistent image, idea, or desire that dominates a person's thoughts or feelings.
Selective serotonin reuptake inhibitors (SSRIs) —A class of antidepressants that work by blocking the reabsorption of serotonin in the brain, thus raising the levels of serotonin. SSRIs include fluoxetine (Prozac), sertraline (Zoloft), and paroxetine (Paxil).
Serotonin —A widely distributed neurotransmitter that is found in blood platelets, the lining of the digestive tract, and the brain, and that works in combination with norepinephrine. It causes very powerful contractions of smooth muscle and is associated with mood, attention, emotions, and sleep. Low levels of serotonin are associated with depression.
Resources
BOOKS
Herbert, Fredrick B. "Obsessive-Compulsive Disorder in Children and Adolescents." In Psychiatric Secrets. Edited by James L. Jacobson et al. Philadelphia: Hanley and Belfus, 2001.
Stafford, Brian, et al. "Anxiety Disorders." In Nelson Textbook of Pediatrics. Edited by Richard E. Behrman et al. Philadelphia: Saunders, 2004.
PERIODICALS
Barrett, P. "Cognitive-behavioral family treatment of childhood obsessive-compulsive disorder: a controlled trial." Journal of the American Academy of Child and Adolescent Psychiatry 43 (January 2004): 46–62.
Storch, E. A. "Behavioral treatment of a child with PANDAS." Journal of the American Academy of Child and Adolescent Psychiatry 86 (May 2004): 510–1.
ORGANIZATIONS
Anxiety Disorders Association of America. 11900 Park Lawn Drive, Suite 100, Rockville, MD 20852. Web site: http://www.adaa.org.
National Alliance for the Mentally Ill (NAMI). Colonial Place Three, 2107 Wilson Blvd., Suite 300, Arlington, VA 22201–3042. Web site: http://www.nami.org.
National Anxiety Foundation. 3135 Custer Dr., Lexington, KY 40517. Web site: http://www.lexington-on-line.com/naf.html.
Carol A. Turkington Rosalyn Carson-DeWitt, MD