Lyme disease
Definition
Lyme disease is an inflammatory disease transmitted through the bite of a deer tick carrying the spiral-shaped bacterium Borrelia burgdorferi . Symptoms can include skin rash, joint inflammation, fever , headache , fatigue, and muscle pain . Lyme disease is also called Lyme borreliosis.
Description
Lyme disease is an inflammatory, systemic disease, meaning that it affects multiple body systems. Although clinical signs of Lyme disease have been reported for more than 100 years, the disease was not recognized as a distinct illness until 1975, when a cluster of unusual arthritis cases in Lyme, Connecticut, led physicians to discover that town residents living near heavily wooded areas were most affected by arthritis and other symptoms. Tick bites were then linked to the cause of the arthritis cases. Borrelia burgdorferi , the spiral-shaped bacterium called a spirochete, that causes Lyme disease, was not discovered until 1981 by Willy Burgdorfer.
Although Lyme disease is easily treated, it is not easily diagnosed, since symptoms are often attributed to other conditions. If not treated early and properly with antibiotics , Lyme disease can have long-term and disabling effects. In its early stages, Lyme disease affects the skin and produces flu-like symptoms; the disease spreads to the joints and nervous system in its later stages.
Transmission
Lyme disease is a vector-borne disease, meaning that it is transmitted from one host to another by a carrier—called a vector—that transmits but does not become infected with the disease. In the United States, the deer tick in the genus Ixodes is the vector for Borrelia burgdorferi and Lyme disease transmission. Lyme disease is transmitted when a tick carrying the Borrelia burgdorferi bacterium bites a human to feed on blood. The bacterium is transferred from the intestines of the tick through the mouthparts and into the bloodstream while the tick is feeding. Ticks are most likely to transmit Borrelia burgdorferi after remaining attached and feeding for two or more days. In most areas, ticks are most active from April to October, but in milder climates, ticks may bite year-round.
During their two-year life cycle and three life stages (larva, nymph, and adult), deer ticks feed on a number of mammals that may carry the Borrelia burgdorferi bacterium in their blood, but the white-footed mouse is the most common source of infection. In the summer, the larval ticks hatch from eggs laid in the ground and feed by attaching themselves to small animals and birds. At this stage, they are not a problem for humans. It is the next stage—the nymph—that causes most cases of Lyme disease. Nymphs are very active from spring through early summer, at the height of outdoor activity for most people. Because they are still quite small (less than 2 mm), they are difficult to spot, giving them ample opportunity to transmit Borrelia burgdorferi while feeding. Although far more adult ticks than nymphs carry Borrelia burgdorferi , the adult ticks are much larger, more easily noticed, and more likely to be removed before they have fed long enough to transmit Borrelia burgdorferi . Neither Borrelia burgdorferi nor Lyme disease can be transmitted directly from one person to another or from pets to humans.
Demographics
Lyme disease is the most common vector-borne disease in the United States. In 2002 alone, 23,763 cases were reported to the Centers for Disease Control and Prevention (CDC), a 40-percent increase over the number reported in 2001. According to the CDC, the actual number of Lyme cases may exceed 200,000 due to underreporting and limitations in disease surveillance methods. CDC statistics indicate that the largest proportion of Lyme disease cases occurs in children aged five to 14 years, and more than 50 percent of Lyme disease cases involve children under age 12. Although cases of Lyme disease have been reported in 49 of the 50 states, more than 95 percent of reported cases occur in just twelve states: Connecticut, Rhode Island, New York, Pennsylvania, Delaware, New Jersey, Maryland, Maine, New Hampshire, Minnesota, Massachusetts, and Wisconsin. In the United States, the Great Lakes region and the Pacific Northwest also have a higher incidence of Lyme disease. The disease is also found in Scandinavia, continental Europe, the countries of the former Soviet Union, Japan, China, and Australia.
Causes and symptoms
Lyme disease is caused by the Borrelia burgdorferi bacterium. Once Borrelia burgdorferi gains entry to the body through a tick bite, it can move through the bloodstream quickly. Only 12 hours after entering the bloodstream, Borrelia burgdorferi can be found in cerebrospinal fluid (which means it can affect the nervous system). Treating Lyme disease early and thoroughly is important because Lyme disease can hide for long periods within the body in a clinically latent state. That ability explains why symptoms can recur in cycles and can flare up after months, years, or decades.
Lyme disease is usually described in terms of length of infection (time since the person was bitten by a tick infected with Lyme disease) and whether Borrelia burgdorferi is localized or disseminated (spread through the body by fluids and cells carrying Borrelia burgdorferi ). Furthermore, when and how symptoms of Lyme disease appear can vary widely from patient to patient. People who experience recurrent bouts of symptoms over time are said to have chronic Lyme disease.
Early localized Lyme disease
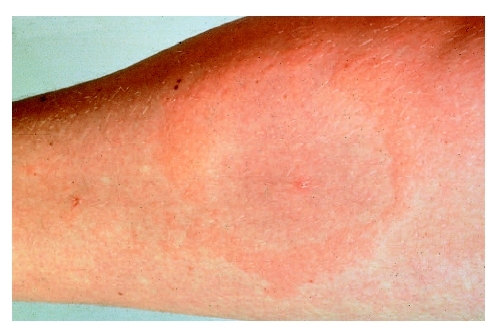
The most recognizable indicator of Lyme disease is a rash around the site of the tick bite. Often, the tick exposure has not been recognized. The eruption might be warm or itch. The rash—erythema migrans (EM)—generally develops within three to 30 days and usually begins as a round, red patch that expands outward from the tick bite. About 80 percent of patients with Lyme disease develop EM. Clearing may take place from the center out, leaving a bull's-eye effect; in some cases, the center gets redder instead of clearing. On children with dark skin, the rash may look like a bruise. Of those who develop Lyme disease, about 50 percent notice flu-like symptoms, including fatigue, headache, chills and fever, muscle and joint pain, and lymph node swelling. Many children with Lyme disease can develop neurologic symptoms within a few weeks following a tick bite. Neurologic symptoms in children with early Lyme disease include dizziness , stiff neck, unilateral or bilateral facial palsy, inflammation of brain membranes (a form of meningitis ), knee and/or wrist arthralgia, tingling/numbness, sleep disturbance, and difficulties with memory, concentration, and learning.
Late disseminated disease and chronic Lyme disease
Weeks, months, or even years after an untreated tick bite, symptoms can appear in several forms, including the following:
- fatigue, forgetfulness, confusion, mood swings, irritability, numbness
- neurologic problems, such as pain (unexplained and not triggered by an injury), Bell's palsy (facial paralysis, usually one-sided but possibly on both sides), a mimicking of the inflammation of brain membranes known as meningitis fever, and severe headache
- arthritis (short episodes of pain and swelling in joints) and other musculoskeletal complaints (Arthritis eventually develops in about 60 percent of patients with untreated Lyme disease.)
In adults, less common effects of Lyme disease are heart abnormalities (such as irregular rhythm or cardiac block) and eye abnormalities (such as swelling of the cornea, tissue, or eye muscles and nerves). However, children with Lyme disease frequently complain of chest pain and have papilledema (swelling of the optic nerve). In addition, children with late-stage Lyme disease are more likely than adults to have fever and joint swelling and pain.
When to call the doctor
A child should see a doctor if an attached tick is found that is engorged with blood (usually indicating attachment for more than six hours). Parents should remove the tick gently with tweezers. Medical laboratories can test the tick for Borrelia burgdorferi if the tick is alive; parents should place the tick in a tightly sealed plastic bag or small bottle with a moistened cotton ball and take it to the doctor. Most doctors will not prescribe antibiotics immediately following a tick bite but will ask parents to monitor their child for symptoms of early Lyme disease.
Less than 50 percent of children realize that they have been bitten by a tick. And, according to pediatricians specializing in Lyme disease, many children already have chronic Lyme disease when they are first diagnosed because children have difficulties effectively verbalizing their symptoms and their symptoms may be misdiagnosed. Any child that develops a round, bull'seye skin rash, joint pain, flu-like symptoms, and/or neurologic symptoms as described above should see a doctor. Because many children do not develop a rash or the rash may not be readily visible (e.g., on the scalp under hair), children living in or visiting areas with a high incidence of Lyme disease and those participating in frequent outdoor activities during active tick months who develop joint pain and neurologic symptoms should see a doctor.
Diagnosis
In children, symptoms of Lyme disease can mimic those of other common childhood conditions, and children may not realize they have been bitten by a tick; therefore, diagnosis of Lyme disease in children can be difficult. Therefore, diagnosis of Lyme disease relies on information the patient and parents provide and the doctor's clinical judgment, particularly through elimination of other possible causes of the symptoms. Differential diagnosis (distinguishing Lyme disease from other diseases) is based on clinical evaluation with laboratory tests used for clarification when necessary. A two-test approach is common to confirm the results. Because of the potential for misleading results (false-positive and false-negative), laboratory tests alone cannot establish the diagnosis.
In February 1999 the Food and Drug Administration (FDA) approved a new blood test for Lyme disease called PreVue. The test, which searches for antigens (substances that stimulate the production of antibodies) produced by Borrelia burgdorferi , gives results within one hour in the doctor's office. A positive result from the PreVue test is confirmed by a second blood test known as the Western blot, which must be done in a laboratory.
Doctors generally know which disease-causing organisms are common in their geographic area. The most helpful piece of information is whether a tick bite or rash was noticed and whether it happened locally or while traveling. Doctors may not consider Lyme disease if it is rare locally but will take it into account if a patient mentions vacationing in an area where the disease is commonly found.
Treatment
The treatment for Lyme disease is antibiotic therapy. If a child has strong indications of Lyme disease (symptoms and medical history), the doctor will probably begin treatment on the presumption of this disease. The American College of Physicians recommends treatment for a patient with a rash resembling EM or who has arthritis, a history of an EM-type rash, and a previous tick bite.
The benefits of early treatment must be weighed against the risks of overtreatment. The longer a patient is ill with Lyme disease before treatment, the longer the course of therapy must be, and the more aggressive the
For most children, oral antibiotics (amoxicillin) are prescribed for 21 days. When symptoms indicate nervous system involvement or a severe episode of Lyme disease, an intravenous antibiotic (ceftriaxone, cefotaxime, ampicillin) may be given for four to six weeks or longer. Some physicians consider intravenous ceftriaxone the best therapy for any late manifestation of disease, but treatments for late Lyme disease are still controversial as of 2004. Corticosteroids (oral) may be prescribed if eye abnormalities occur, but they should not be used without first consulting an eye doctor. Nonsteroidal anti-inflammatory medications (ibuprofen) may be prescribed for joint pain and inflammation.
The doctor may have to adjust the treatment regimen or change medications based on the patient's response. Treatment can be difficult because Borrelia burgdorferi comes in several strains (some may react to different antibiotics than others) and may even have the ability to switch forms during the course of infection. Also, Borrelia burgdorferi can shut itself up in cell niches, allowing it to hide from antibiotics. Finally, antibiotics can kill Borrelia burgdorferi only while it is active rather than dormant.
Alternative treatment
Supportive therapies may minimize symptoms of Lyme disease or improve the immune response. These include vitamin and nutritional supplements, mostly for chronic fatigue and increased susceptibility to infection. For example, yogurt and Lactobacillus acidophilus preparations help fight yeast infections, which are common in patients on long-term antibiotic therapy. In addition, botanical medicine and homeopathy can be considered to help bring the body's systems back to a state of health and well-being. A Western herb, spilanthes ( Spilanthes spp.), may be effective in treating diseases such as Lyme disease that are caused by spirochetes (spiral-shaped bacteria). Therapy using a low-current electrical field or magnetic pulses is also as of 2004 under research to treat bacterial infections. It is important to note that no alternative treatments have been proven to cure Lyme disease.
Prognosis
If aggressive antibiotic therapy is given early and the patient cooperates fully and sticks to the medication schedule, recovery should be complete. Only a small percentage of Lyme disease patients fail to respond or relapse (have recurring episodes). Most long-term effects of the disease result when diagnosis and treatment is delayed or missed. Co-infection with other infectious organisms spread by ticks in the same areas as Borrelia burgdorferi (babesiosis and ehrlichiosis, for instance) may be responsible for treatment failures or more severe symptoms. Most fatalities reported with Lyme disease involved patients coinfected with babesiosis.
Prevention
Lyme disease can be prevented by taking the following measures to reduce exposure to tick bites:
- Avoid areas likely to be infested with ticks, especially during spring and summer, when tick nymphs are most likely to feed. Areas most likely to be infested with ticks include moist and shady areas, wooded and brushy areas, overgrown grassy areas, and areas with a high rodent and deer population.
- When outdoors, wear light-colored clothing, long-sleeved shirts, and long pants tucked into socks or boots.
- Use insect repellents according to safety guidelines for children.
- Perform a full-body "tick check" after outdoor activities and use tweezers to gently remove and dispose of ticks.
- Do not try to remove the tick by using petroleum jelly, alcohol, or a lit match.
- Place the tick in a closed container (for species identification later, should symptoms develop) or dispose of it by flushing or by placing the tick between scotch tape.
- Check pets frequently for ticks, since ticks can migrate to children from pets.
Update on vaccination
A vaccine for Lyme disease known as LYMErix was available from 1998 to 2002, when it was removed from the United States market. The decision was influenced by reports that LYMErix may be responsible for neurologic complications in vaccinated patients. As of late 2004, the best prevention strategy was minimizing risk of exposure to ticks and using personal protection precautions.
KEY TERMS
Babesiosis —A infection transmitted by the bite of a tick and characterized by fever, headache, nausea, and muscle pain.
Bell's palsy —Facial paralysis or weakness with a sudden onset, caused by swelling or inflammation of the seventh cranial nerve, which controls the facial muscles. Disseminated Lyme disease sometimes causes Bell's palsy.
Blood-brain barrier —An arrangement of cells within the blood vessels of the brain that prevents the passage of toxic substances, including infectious agents, from the blood and into the brain. It also makes it difficult for certain medications to pass into brain tissue.
Cerebrospinal fluid —The clear, normally colorless fluid that fills the brain cavities (ventricles), the subarachnoid space around the brain, and the spinal cord and acts as a shock absorber.
Disseminated —Spread to other tissues.
Erythema migrans —A red skin rash that is one of the first signs of Lyme disease in about 75% of patients.
Lyme borreliosis —Another name for Lyme disease.
Spirochete —A type of bacterium with a long, slender, coiled shape. Syphilis and Lyme disease are caused by spirochetes.
Vector —A carrier organism (such as a fly or mosquito) which serves to deliver a virus (or other agent of infection) to a host. Also refers to a retrovirus that had been modified and is used to introduce specific genes into the genome of an organism.
Parental concerns
Because most children do not realize they have been in tick-infested areas or been bitten by a tick and because deer ticks can be the size of a poppy seed or smaller, parents should be diligent about checking children for ticks, especially if the family lives in or visits an area with a high incidence of Lyme disease or an area near tick habitats. Also, because Lyme disease is difficult to diagnose in children, parents who suspect Lyme disease in their children should inform their doctor about the possibility of the disease and be proactive in requesting further medical evaluation and treatment.
Resources
BOOKS
"Bacterial Diseases Caused by Spirochetes: Lyme Disease (Lyme Borreliosis)." Section 13, Chapter 157 in The Merck Manual of Diagnosis and Therapy. Edited by Mark H. Beers and Robert Berkow. Whitehouse Station, NJ: Merck Research Laboratories, 2002.
Stewart, Gail B. Lyme Disease. Indianapolis, IN: Lucent Books, 2003.
PERIODICALS
Bryant, K. A., and Marshall G. S. "Clinical Manifestations of Tick-Borne Infections in Children." Clinical and Diagnostic Laboratory Immunology 7 (July 2000): 523–27.
Krupp, et al. "Study and Treatment of Post Lyme Disease (STOP-LD): A Randomized Double Masked Clinical Trial." Neurology 60 (June 24, 2003): 1923–30.
Nachman, S. A., and L. Pontrelli. "Central Nervous System Lyme Disease." Seminars in Pediatric Infectious Diseases 14 (April 2003): 123–30.
Pavia, C. S. "Current and Novel Therapies for Lyme Disease." Expert Opinion on Investigational Drugs 12 (June 2003): 1003–16.
Wormser, G. P., et al. "Duration of Antibiotic Therapy for Early Lyme Disease: A Randomized, Double-Blind, Placebo-Controlled Trial." Annals of Internal Medicine 138 (May 6, 2003): 697–704.
ORGANIZATIONS
Centers for Disease Control and Prevention. 1600 Clifton Rd., NE, Atlanta, GA 30333. Web site: http://www.cdc.gov.
Lyme Disease Foundation. One Financial Plaza, Hartford, CT 06103. Web site: http://www.lyme.org.
Lyme Disease Network of New Jersey Inc. 43 Winton Road, East Brunswick, NJ 08816. Web site: http://www.lymenet.org.
National Institute of Allergy and Infectious Diseases (NIAID). 31 Center Drive, Room 7A50 MSC 2520, Bethesda, MD 20892. Web site: http://www.niaid.nih.gov.
WEB SITES
"CDC Lyme Disease Home Page." Centers for Disease Control and Prevention, Division of Vector-Borne Infectious Diseases. Available online at http://www.cdc.gov/ncidod/dvbid/lyme (accessed November 21, 2004).
"Children's Corner." Lyme Disease Foundation. Available online at http://www.lyme.org/children.html(accessed November 21, 2004).
Edlow, Jonathan A. "Tick-Borne Diseases, Lyme." eMedicine , December 13, 2002. Available online at http://www.emedicine.com/emerg/topic588.htm (accessed November 21, 2004).
"Neurological Manifestations of Lyme Disease in Children." LymeNet. Available online at http://library.lymenet.org (accessed November 21, 2004).
Jennifer E. Sisk, MA
Comment about this article, ask questions, or add new information about this topic: