Lead poisoning
Definition
Lead poisoning occurs when a person swallows, absorbs, or inhales lead in any form. The result can be damaging to the brain, nerves, and many other parts of the body. Acute lead poisoning, which is somewhat rare, occurs when a relatively large amount of lead is taken into the body over a short period of time. Chronic lead poisoning is a common problem in children that occurs when small amounts of lead are ingested over a longer period. The Centers for Disease Control and Prevention (CDC) defines childhood lead poisoning as a whole-blood lead concentration equal to or greater than 10 micrograms/dL.
Description
Lead can damage almost every system in the human body, and it can also cause high blood pressure ( hypertension ). It is particularly harmful to the developing brain of fetuses and young children. The higher the level of lead in a child's blood and the longer this elevated level lasts, the greater the chance of ill effects. Over the long term, lead poisoning in a child can lead to learning disabilities, behavioral problems, and even mental retardation . At very high levels, lead poisoning can cause seizures, coma, and even death.
Many children with elevated blood levels are exposed to lead through peeling paint in older homes. Others are exposed through dust or soil that has been contaminated by old paint or past emissions of leaded gasoline. Since children between the ages of 12 and 36 months are apt to put things in their mouths, they are more likely than older children to take in lead. Pregnant women who come into contact with lead can pass it along to the fetus.
Over 80 percent of American homes built before 1978 have lead-based paint in them, according to the Centers for Disease Control and Prevention (CDC). The older the home, the more likely it is to contain lead paint, and the higher the concentration of lead in the paint is apt to be. Some homes also have lead in the water pipes or plumbing. Without knowing it, people may have lead in the paint, dust, or soil around their homes or in their drinking water, since lead cannot be seen, smelled, or tasted. Because lead does not break down naturally, it can continue to cause problems until it is removed.
Demographics
According to the Agency for Toxic Substances and Disease Registry, approximately one out of every six children in the United States has a high level of lead in the blood. According to the National Center for Environmental Health, there were about 200 deaths from lead poisoning in the United States between 1979 and 1998. Most of the deaths were among males (74%), African Americans (67%), adults over the age of 45 (76%), and Southerners (70%).
Causes and symptoms
Before scientists knew how harmful it could be, lead was widely used in paint, gasoline, water pipes, and many other products. In the early 2000s house paint is almost lead-free, gasoline is unleaded, and household plumbing is no longer made with lead materials. Still, remnants of the old hazards remain. Following are some sources of lead exposure:
- Lead-based paint: This is the most common source of exposure to large amounts of lead among preschoolers. Children may eat paint chips from older homes that have fallen into disrepair. They may also chew on painted surfaces such as windowsills. In addition, paint may be disturbed during remodeling.
- Dust and soil: These can be contaminated with lead from old paint or past emissions of leaded gasoline. In addition, pollution from operating or abandoned industrial sites and smelters can find its way into the soil, resulting in soil contamination.
- Drinking water: Exposure may come from lead water pipes, found in many homes built before 1930. Even newer copper pipes may have lead solder. Also, some new homes have brass faucets and fittings that can leach lead.
-
Jobs and hobbies: A number of activities can expose participants to
lead. These include making pottery or stained glass, refinishing
furniture, doing home repairs,
and using indoor firing ranges. When adults take part in such activities, they may inadvertently expose children to lead residue that is on their clothing or on scrap materials.
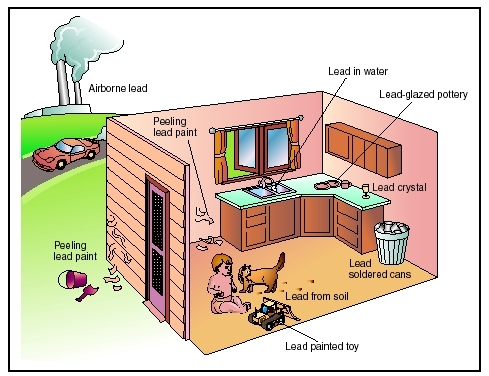 Continuous exposure to lead can damage nearly every system in the human body and is particularly harmful to the developing brain of fetuses and young children. Common sources of lead exposure include lead-based paint, dust and soil, drinking water, food from cans, and eating utensils, such as plates and drinking glasses, that are lead-based.(Illustration by Electronic Illustrators Group.)
Continuous exposure to lead can damage nearly every system in the human body and is particularly harmful to the developing brain of fetuses and young children. Common sources of lead exposure include lead-based paint, dust and soil, drinking water, food from cans, and eating utensils, such as plates and drinking glasses, that are lead-based.(Illustration by Electronic Illustrators Group.) - Food: Imported food cans often have lead solder. Lead may also be found in leaded crystal glassware and some imported ceramic or old ceramic dishes (e.g., ceramic dishes from Mexico). A 2003 study of cases of lead poisoning in pregnant women found that 70 percent of affected people were Hispanics, most of whom had absorbed the lead from their pottery. In addition, food may be contaminated by lead in the water or soil.
- Folk medicines: Certain folk medicines (for example, alarcon, alkohl, azarcon, bali goli, coral, ghasard, greta, liga, pay-loo-ah, and rueda) and traditional cosmetics (kohl, for example) contain high concentrations of lead.
- Moonshine whiskey: Lead poisoning from drinking illegally distilled liquor is still a cause of death among adults in the southern United States.
- Gunshot wounds : Toxic amounts of lead can be absorbed from bullets or bullet fragments that remain in the body after emergency surgery.
Evidence as of 2004 suggested that lead may be harmful to children even at low levels that were once thought to be safe, and the risk of damage rises as blood levels of lead increase. The symptoms of chronic lead poisoning take time to develop, however. Children can appear healthy despite having high levels of lead in their blood. Over time, though, problems such as the following may arise:
- learning disabilities
- hyperactivity
- mental retardation
- slowed growth
- hearing loss
- headaches
It is also known that certain genetic factors increase the harmful effects of lead poisoning in susceptible children; however, these factors are not completely understood.
Lead poisoning is also harmful to adults, in whom it can cause high blood pressure, digestive problems, nerve disorders, memory loss, and muscle and joint pain . In addition, it can lead to difficulties during pregnancy, as well as cause reproductive problems in both men and women.
In the early 2000s, chronic exposure to lead in the environment has been found to speed up the progression of kidney disorders in people without diabetes.
Acute lead poisoning
Acute lead poisoning, while less common, shows up more quickly and can be fatal. Symptoms such as the following may occur:
- severe abdominal pain
- diarrhea
- nausea and vomiting
- weakness of the limbs
- seizures
- coma
When to call the doctor
The CDC recommends testing all children at 12 months of age and, if possible, again at 24 months. Testing should start at six months for children at risk for lead poisoning.
Diagnosis
A high level of lead in the blood can be detected with a simple blood test. In fact, testing is the only way to know for sure if children without symptoms have been exposed to lead, since they can appear healthy even as long-term damage occurs. Based on test results and a child's risk factors, the doctor will then decide whether further testing is needed and how often. In some states, more frequent testing is required by law.
Children at risk
Children with an increased risk of lead poisoning include those for whom the following is true:
- They live in or regularly visit a house built before 1978 in which chipped or peeling paint is present.
- They live in or regularly visit a house that was built before 1978 where remodeling is planned or underway.
- They have a brother or sister, housemate, or playmate who has been diagnosed with lead poisoning.
- They have the habit of eating dirt or have been diagnosed with pica.
- They live with an adult whose job or hobby involves exposure to lead.
- They live near an active lead smelter, battery-recycling plant, or other industry that can create lead pollution.
Adults at risk
Testing is also important for adults whose job or hobby puts them at risk for lead poisoning. This need applies to people who take part in the following activities:
- glazed pottery or stained glass production
- furniture refinishing
- home renovation
- target shooting at indoor firing ranges
- battery reclamation
- precious metal refining
- radiator repair
- art restoration
Treatment
The first step in treating lead poisoning is to avoid further contact with lead. For adults, this usually means making changes at work or in hobbies. For children, it means that parents and guardians need to find and remove sources of lead in the home. In most states, the public health department can help assess the home and identify lead sources.
If the problem is lead paint, a professional with special training should remove it. Removal of lead paint is not a do-it-yourself project. Scraping or sanding lead paint creates large amounts of dust that can poison people in the home. This dust can stay around long after the work is completed. In addition, heating lead paint can release lead into the air. For these reasons, lead paint should only be removed by someone who knows how to do the job safely and has the equipment to clean up thoroughly. Occupants, especially children and pregnant women, should leave the home until the cleanup is finished.
Medical professionals should take all necessary steps to remove bullets or bullet fragments from people with gunshot injuries.
If blood levels of lead are high enough, the doctor may also prescribe chelation therapy. This refers to treatment with chemicals that bind to the lead and help the body pass it in urine at a faster rate. There are four chemical agents that may be used for this purpose, either alone or in combination. Edetate calcium disodium (EDTA calcium) and dimercaprol (BAL) are given through an intravenous line or in shots, while succimer (Chemet) and penicillamine (Cuprimine, Depen) are taken by mouth. (Although many doctors prescribe penicillamine for lead poisoning, this use of the drug has not been approved by the Food and Drug Administration.)
Changes in diet are no substitute for medical treatment. However, getting enough calcium, zinc, and protein may help reduce the amount of lead the body absorbs. Iron is also important, since people who are deficient in this nutrient absorb more lead. Garlic and thiamine, a B-complex vitamin, have been used to treat lead poisoning in animals. However, their usefulness in humans for this purpose has not as of 2004 been demonstrated. Nutritional, botanical, and homeopathic medicines can be administered once the source is removed to help correct any imbalances brought on by lead toxicity.
Prognosis
If acute lead poisoning reaches the stage of seizures and coma, there is a high risk of death. Even if the person survives, there is a good chance of permanent brain damage. The long-term effects of lower levels of lead can also be permanent and severe. However, if chronic lead poisoning is caught early, these negative effects can be limited by reducing future exposure to lead and getting proper medical treatment.
Prevention
Many cases of lead poisoning can be prevented. The following steps can help:
KEY TERMS
Chelation therapy —A treatment using chelating agents, compounds that surround and bind to target substances allowing them to be excreted from the body.
Dimercaprol —A chemical agent used to remove excess lead from the body.
Edetate calcium disodium —A chemical chelating agent used to remove excess lead from the body.
Penicillamine (Cuprimine, Depen) —A drug used to treat medical problems (such as excess copper in the body and rheumatoid arthritis) and to prevent kidney stones. It is also sometimes prescribed to remove excess lead from the body.
Pica —A desire that sometimes arises in pregnancy to eat nonfood substances, such as dirt or clay.
Succimer —A chelating agent that is used to remove excess lead from the body. Sold under the trade name Chemet.
- Keep the areas where children play as clean and dust-free as possible.
- Wash pacifiers and bottles when they fall to the floor and wash stuffed animals and toys often.
- Make sure children wash their hands before meals and at bedtime.
- Mop floors and wipe windowsills and other chewable surfaces, such as cribs, twice a week with a solution of powdered dishwasher detergent in warm water.
- Plant bushes next to an older home with painted exterior walls to keep children at a distance.
- Plant grass or another ground cover in soil that is likely to be contaminated, such as soil around a home built before 1960 or located near a major highway.
- Have household tap water tested to find out if it contains lead.
- Use only water from the cold-water tap for drinking, cooking, and making baby formula, since hot water is likely to contain higher levels of lead.
- If the cold water has not been used for six hours or more, run it for several seconds, until it becomes as cold as it will get, before using it for drinking or cooking. The more time water has been sitting in the pipes, the more lead it may contain.
- Do not store food in open cans, especially imported cans.
- Do not store or serve food in pottery meant for decorative use.
- People who work with lead in a job or hobby should change their clothes before they go home.
Nutritional concerns
Avoid preparing or serving food in containers that have lead in their glazing. Do not consume homemade liquor that has been distilled.
Parental concerns
Lead tastes sweet. Parents living in homes built prior to 1978 should be vigilant regarding removing all flaking or peeling paint. Simply re-painting such surfaces will not resolve the problem. Parents must monitor the environments in which their children play and the objects that go into their children's mouths. Cleanliness is a must if old paint is in a child's environment. Removal (stripping paint to bare metal or bare wood) of lead is the best way to prevent lead exposure in children.
Resources
BOOKS
Goto, Collin S. "Heavy Metal Intoxication." In Nelson Textbook of Pediatrics , 17th ed. Edited by Richard E. Behrman, et al. Philadelphia: Saunders, 2003, pp. 2355–7.
Gupta, S. K., et al. Emergency Toxicology: Management of Common Poisons. Boca Raton, FL: CRC Press, 2003.
Klaasen, Curtis D., and John Doull. Casarett and Doull's Toxicology: The Basic Science of Poisons , 6th ed. New York: McGraw Hill, 2001.
Markowitz, Morrie. "Lead Poisoning." In Nelson Textbook of Pediatrics , 17th ed. Edited by Richard E. Behrman, et al. Philadelphia: Saunders, 2003, pp. 2358–61.
PERIODICALS
Clark, S., et al. "The influence of exterior dust and soil lead on interior dust lead levels in housing that had undergone lead-based paint hazard control." Journal of Occupational and Environmental Hygiene 1, no. 5 (2004): 273–82.
Dietert, R. R., et al. "Developmental immunotoxicology of lead." Toxicology and Applied Pharmacology 198, no. 2 (2004): 86–94.
Dorea, J. G. "Mercury and lead during breast-feeding." British Journal of Nutrition 92, no. 1 (2004): 21–40. Kwong W. T., et al. "Interactions between iron deficiency and lead poisoning: epidemiology and pathogenesis." Science of the Total Environment 330, no. 1–3 (2004): 21–37.
Sandel, M., et al. "The effects of housing interventions on child health." Pediatric Annals 33, no. 7 (2004): 474–81.
Stretesky, P. B., and M. J. Lynch. "The relationship between lead and crime." Journal of Health and Social Behavior 45, no. 2 (2004): 214–29.
ORGANIZATIONS
American Academy of Clinical Toxicology. 777 East Park Drive, PO Box 8820, Harrisburg, PA 17105–8820. Web site: http://www.clintox.org/index.html.
American Academy of Family Physicians. 11400 Tomahawk Creek Parkway, Leawood, KS 66211–2672. Web site: http://www.aafp.org/.
American Academy of Pediatrics. 141 Northwest Point Boulevard, Elk Grove Village, IL 60007–1098. Web site: http://www.aap.org/default.htm.
American Association of Poison Control Centers. 3201 New Mexico Avenue NW, Washington, DC 20016. Web site: http://www.aapcc.org/.
American College of Occupational and Environmental Medicine. 55 West Seegers Road, Arlington Heights, IL 60005. Web site: http://www.acoem.org/.
WEB SITES
"CDC Childhood Lead Poisoning Prevention Program: Spotlight on Lead." Centers for Disease Control and Prevention. Available online at http://www.cdc.gov/nceh/lead/lead.htm and http://www.cdc.gov/nceh/lead/factsheets/leadfcts.htm (accessed November 11, 2004).
"Lead-based Paint Hazard Control Grant Program." U.S. Department of Housing and Urban Development. Available online at http://www.hud.gov/offices/lead/ (accessed November 11, 2004).
"Lead in Paint, Dust, and Soil." U.S. Environmental Protection Agency. Available online at http://www.epa.gov/lead/ (accessed November 11, 2004).
"Lead Poisoning." National Library of Medicine. Available online at http://www.nlm.nih.gov/medlineplus/leadpoisoning.html (accessed November 11, 2004).
"Occupational Lead Poisoning." American Academy of Family Physicians. Available online at http://www.aafp.org/afp/980215ap/stauding.html (accessed November 11, 2004).
L. Fleming Fallon, Jr., MD, DrPH
Comment about this article, ask questions, or add new information about this topic: