Electroencephalogram
Definition
An electroencephalogram (EEG), also called a brain wave test, is a diagnostic test which measures the electrical activity of the brain (brain waves) using highly sensitive recording equipment attached to the scalp by fine electrodes.
Purpose
EEG is performed to detect abnormalities in the electrical activity of the brain which may help diagnose the presence and type of various brain disorders, to look for causes of confusion, and to evaluate head injuries, tumors, infections, degenerative diseases, and other disturbances that affect the brain. The test is also used to investigate periods of unconsciousness. EEG may also confirm brain death in someone who is in a coma. EEG cannot be used to measure intelligence or diagnose mental illness. Specifically, EEG is used to diagnose the following:
- seizure disorders (such as epilepsy or convulsions)
- structural brain abnormality (such as a brain tumor or brain abscess)
- head injury, encephalitis (inflammation of the brain)
- hemorrhage (abnormal bleeding caused by a ruptured blood vessel)
- cerebral infarct (tissue that is dead because of a blockage of the blood supply)
- sleep disorders (such as narcolepsy)
Description
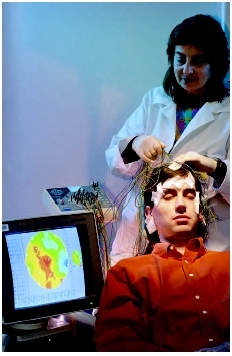
Brain cells communicate by producing tiny electrical impulses, also called brain waves. These electrical signals have certain rhythms and shapes, and EEG is a technique that measures, records, and analyzes these signals to help make a diagnosis. Electrodes are used to detect the electrical signals. They come in the shape of small discs that are applied to the head and connected to a recording device. The recording machine then converts the electrical signals into a series of wavy lines that are drawn onto a moving piece of graph paper. An EEG test causes no discomfort. Although having electrodes pasted on the skin may feel strange, they only record activity and do not produce any sensation. The patient needs to lie still with eyes closed because any movement can affect results. The patient may also be asked to do certain things during the EEG recording, such as breathing deeply and rapidly for several minutes or looking at a bright flickering light.
An EEG is performed by an EEG technician in a specially designed room that may be in the doctor's office or at a hospital. The patient is asked to lie on a bed or in a comfortable chair so that a relaxed EEG recording can be done. The technician either measures the scalp and marks the spots where small discs (electrodes) will be placed or fits the head with a special cap containing between 16 and 25 of these discs. The scalp is then rubbed with a mild, scratchy cleanser that may cause mild discomfort for a short while. The discs are attached to the body with a cream or gel. Alternatively, the technician may secure the discs to the skin with an adhesive. The heart may also be monitored during the procedure.
Precautions
Before an EEG, care should be taken to avoid washing hair with an oily scalp product 24 hours before the test. Doctors usually recommend that patients eat a meal or light snack some four hours before the test. Caffeinated drinks should be avoided for eight hours before the test. Sometimes, the EEG gives better results when the patient has had less than the usual amount of sleep. The doctor may ask that the child be kept awake for all or part of the night before the EEG. The healthcare provider may also discontinue some medications before the test.
Preparation
The physical and psychological preparation required for this test depends on the child's age, interests, previous experiences, and level of trust. For older children, research has shown that preparing ahead can reduce crying or resisting the test. In addition, children report less pain and show less distress when prepared. Proper preparation for the test can reduce a child's anxiety , encourage cooperation, and help develop coping skills.
Some general guidelines for preparing a toddler or preschooler for an EEG include the following:
- Explain the EEG procedure in words that the child understands, avoiding abstract terminology.
- Ensure that the child understands the exact body part involved and that the procedure will be limited to that area.
- Describe how the test is likely to feel.
- Give the child permission to yell, cry, or otherwise express any pain or discomfort verbally.
- Stress the benefits of the EEG procedure and list things that the child may find pleasurable after the test, such as feeling better or going home.
The above guidelines also apply to school age children. Additionally, for older children, parents can try the following:
- Suggest ways to keep calm and reduce anxiety such as counting, deep breathing, or thinking pleasant thoughts.
- Include the child in the decision-making process, such as the time of day where the EEG is performed.
- Suggest that the child hold the hand of the technician or someone else helping with the procedure.
As for adolescents, detailed information about the EEG should be provided and the reasons for the procedure should be explained in correct medical terminology. When the EEG is required for a seizure disorder , there is the potential risk that the test will trigger a seizure. This possibility should be openly discussed. Adolescents commonly have high concerns about risks and the best way to prepare them is to fully inform them. The healthcare provider could also be asked to limit the number of
Aftercare
There are no side effects or special procedures required after an EEG. The technician simply removes the gel with water and the adhesive, if used, with a special cleanser. Shampooing will rid the hair of any other material. A few patients are mildly sensitive to the gel or may get irritation from the rubbing of their scalps.
KEY TERMS
Electrode —A medium for conducting an electrical current.
Encephalitis —Inflammation of the brain, usually caused by a virus. The inflammation may interfere with normal brain function and may cause seizures, sleepiness, confusion, personality changes, weakness in one or more parts of the body, and even coma.
Epilepsy —A neurological disorder characterized by recurrent seizures with or without a loss of consciousness.
Hemorrhage —Severe, massive bleeding that is difficult to control. The bleeding may be internal or external.
Hyperventilation —Rapid, deep breathing, possibly exceeding 40 breaths/minute. The most common cause is anxiety, although fever, aspirin overdose, serious infections, stroke, or other diseases of the brain or nervous system. Also refers to a respiratory therapy involving deeper and/or faster breathing to keep the carbon dioxide pressure in the blood below normal.
Narcolepsy —A life-long sleep disorder marked by four symptoms: sudden brief sleep attacks, cataplexy (a sudden loss of muscle tone usually lasting up to 30 minutes), temporary paralysis, and hallucinations. The hallucinations are associated with falling asleep or the transition from sleeping to waking.
Seizure —A sudden attack, spasm, or convulsion.
Sleep disorder —Any condition that interferes with sleep. Sleep disorders are characterized by disturbance in the amount of sleep, in the quality or timing of sleep, or in the behaviors or physiological conditions associated with sleep.
Risks
The EEG test is very safe. However, if a patient has a seizure disorder, a seizure may be triggered by the flashing lights or hyperventilation. The healthcare provider performing the EEG is trained to take care of the patient if this happens.
Normal results
An EEG returns normal results when brain waves have normal frequency and amplitude and other characteristics are typical.
Parental concerns
Before the test, parents should know that the child probably will cry, and restraints may be used. The most important way to help a child through an EEG procedure is by being there and caring. Crying is a normal response to the strange environment, unfamiliar people, restraints, and separation from the parent. Infants and young children will cry more for these reasons than because the test or procedure is uncomfortable. Knowing this from the onset may help parents feel less anxiety about what to expect. Having specific information about the test may further reduce anxiety.
See also Encephalitis ; Narcolepsy ; Sleep disorders .
Resources
BOOKS
Electroencephalogram: A Medical Dictionary, Bibliography, and Annotated Research Guide to Internet. San Diego, CA: Icon Health Publications, 2004.
Shaw, John C. The Brain's Alpha Rhythms and the Mind. New York: Elsevier Science, 2003.
PERIODICALS
Foley, C. M., et al. "Long-term Computer-assisted Outpatient Electroencephalogram Monitoring in Children and Adolescents." Journal of Child Neurology 15, no. 1 (January 2000): 49–55.
Jenny, O. G., and M. A. Carskadon. "Spectral Analysis of the Sleep Electroencephalogram during Adolescence." Sleep 27, no. 4 (June 2004): 774–83.
Nasr, J. T., et al. "The Electroencephalogram in Children with Developmental Dysphasia." Epilepsy Behavior 2, no. 2 (April 2001): 115–18.
Wassmer, E., et al. "Melatonin as a Sleep Inductor for Electroencephalogram Recordings in Children." Clinical Neurophysiology 112, no. 4 (April 2001): 683–85.
ORGANIZATIONS
American Academy of Neurology Foundation. 1080 Montreal Avenue, St. Paul, MN 55116. Web site: http://www.neurofoundation.com.
American Society of Neurophysiological Monitoring. PO Box 60487, Chicago, IL 60660–0487. Web site: http://www.asnm.org.
National Institute of Neurological Disorders and Stroke (NINDS). PO Box 5801, Bethesda, MD 20824. Web site: http://www.ninds.nih.gov.
WEB SITES
"EEG." Medline Plus. Available online at http://www.nlm.nih.gov/medlineplus/ency/article/003931.htm (accessed November 17, 2004).
"The '10–20 System' of Electrode Placement." Available online at http://faculty.Washington.edu/chudler/1020.html (accessed November 17, 2004).
Monique Laberge, Ph.D.
Comment about this article, ask questions, or add new information about this topic: